📋 Quick Summary
- Topic: Childhood peaks, adult and elderly risks, environmental exposures, and how demographics shape leukemia incidence.
- Key Takeaway: Early recognition and medical consultation are critical for the best clinical outcomes.
- Remember: Always consult a qualified healthcare professional if you have concerns.
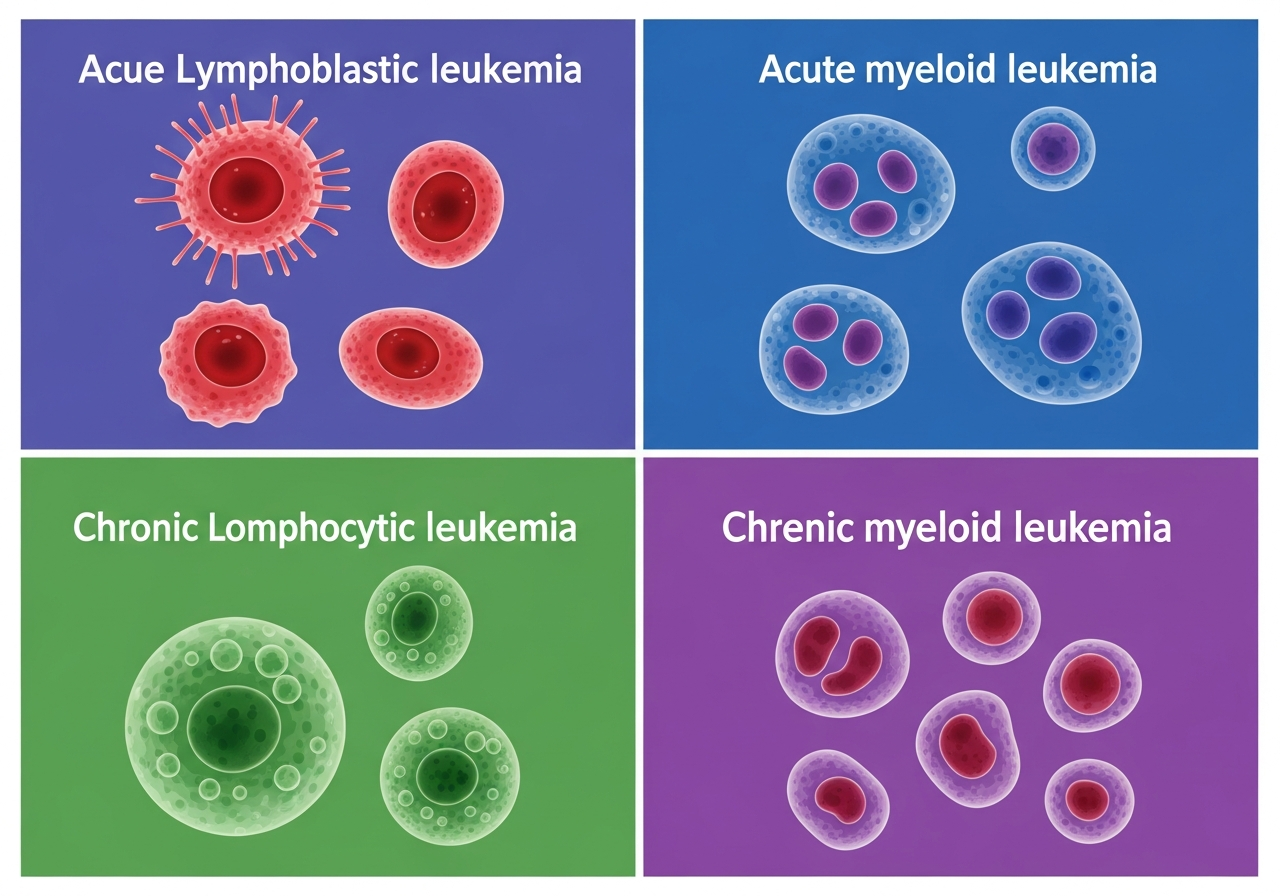
Leukemia Risk Across Life Stages: What You Need to Know
Leukemia does not discriminate by age — it affects infants, children, teenagers, young adults, the middle-aged, and the elderly. However, the risk of developing different types of leukemia varies dramatically across life stages, as do the biological characteristics of the disease, its clinical presentation, and the treatment approach. Understanding which leukemia types are most common at each life stage helps patients and families contextualize a new diagnosis and supports informed conversations with healthcare providers about risk and screening.
In total, approximately 60,000 Americans are diagnosed with leukemia each year. Leukemia is the most common cancer in children under 15, accounting for approximately 30% of all pediatric cancer diagnoses. In adults, leukemia accounts for approximately 3% of new cancer diagnoses — less frequent in absolute terms than in children, but still significant given the larger adult population. Several leukemia types — CLL, AML, CML, and CMML — have incidence that rises steeply with age, making leukemia increasingly prevalent as the population ages.
Leukemia Risk in Infants (Under 1 Year)
Infant leukemia — defined as leukemia diagnosed in the first 12 months of life — is rare but biologically distinctive and clinically urgent. The dominant type is infant ALL, which is biologically unlike older-child ALL in nearly every way:
- More than 80% of infant ALL cases carry rearrangements of the KMT2A (MLL) gene at chromosome 11q23 — a hallmark of aggressive disease
- KMT2A-rearranged infant ALL responds poorly to standard multi-agent chemotherapy; cure rates remain below 50% even with very intensive protocols and transplantation
- Age under 6 months at diagnosis is an independent adverse prognostic factor
- Current research is actively investigating targeted approaches for KMT2A-rearranged infant ALL, including menin inhibitors (revumenib) which show promising early results
Infant AML accounts for a small proportion of infant leukemia cases and includes both KMT2A-rearranged AML (with monocytic differentiation) and the unique entity of Down syndrome-related transient myeloproliferative disorder (TAM) and megakaryoblastic leukemia.
Leukemia Risk in School-Age Children (Ages 3–12)
This age range represents the peak of childhood ALL incidence, with a specific peak between ages 2 and 5. The leukemia biology in this group is remarkably favorable — characterized by high rates of hyperdiploidy (extra chromosomes), ETV6-RUNX1 fusion gene, and other favorable cytogenetic features that respond excellently to standard multi-agent chemotherapy. This is the group in which cure rates exceeding 95% have been achieved.
The reasons for the childhood ALL peak in the 2–5 year range are still not fully understood but likely reflect the period of rapid B-lymphocyte development and education that occurs in early childhood, creating a window of vulnerability for leukemogenic mutations to occur. Environmental exposures during pregnancy and early infancy, including infections and immune stimulation patterns, may influence this risk. The "delayed infection" hypothesis suggests that children with reduced early microbial exposure (born by Caesarean section, not breastfed, limited daycare attendance) may have an altered immune development that paradoxically increases ALL risk — though no intervention based on this hypothesis has been validated.
Leukemia Risk in Adolescents (Ages 13–21)
In adolescents, ALL remains the predominant leukemia type but with several biological shifts from younger childhood:
- T-cell ALL increases as a proportion of cases (15–25% vs. ~10% in younger children)
- Favorable cytogenetics (hyperdiploidy, ETV6-RUNX1) become less common
- The Philadelphia chromosome-like (Ph-like) ALL subtype — characterized by kinase-activating gene fusions but without BCR-ABL1 — increases in frequency
- Outcomes are somewhat worse than in standard-risk younger children, but "pediatric-inspired" intensive regimens (using the same treatment approach as pediatric protocols) produce significantly better outcomes in adolescents and young adults than adult-type regimens
Adolescents with leukemia face unique psychosocial challenges: treatment during a critical period of identity development, peer separation during prolonged therapy, educational disruption, and fertility concerns (adolescent males who receive cytotoxic therapy should be offered sperm banking; adolescent females should discuss ovarian tissue or egg cryopreservation options).
Leukemia Risk in Young Adults (Ages 22–40)
In young adulthood, ALL and AML are the most common leukemia diagnoses. CML is also more common in young and middle-aged adults than in children or elderly populations.
Young adult ALL has become an area of active research and improving outcomes, largely driven by the adoption of pediatric-inspired treatment regimens (CALGB 10403, GRAALL trials) that use higher-dose asparaginase and more intensive consolidation than historical adult ALL protocols. These approaches have improved the 3-year overall survival in young adult ALL from approximately 55% to 70–75% in prospective trials.
AML in young adults is biologically more varied than in older adults, with a higher proportion of favorable molecular subtypes (CBF-AML, NPM1-mutated AML). Allogeneic SCT remains important for intermediate- and high-risk young adult AML because this age group has the physiological reserve to tolerate myeloablative conditioning.
CML in young adults presents important quality-of-life considerations — TKI therapy is highly effective but, in the context of a 40-year treatment horizon for a 30-year-old patient, considerations around medication cost, long-term side effects, and the goal of achieving treatment-free remission are particularly salient. See our CML treatment guide for more on CML management in younger patients.
Leukemia Risk in Middle Age (Ages 40–60)
The transition from young adulthood to middle age marks a shift in leukemia epidemiology. While ALL and AML continue to occur, the incidence of therapy-related AML increases significantly in this age group — driven by survivors of prior cancers (breast cancer, lymphoma) who were treated with alkylating agents or topoisomerase II inhibitors in earlier decades. Secondary AML arising from prior MDS also begins to emerge more commonly.
CML, with its peak incidence in the 40–60 age range, is a significant diagnosis in this group. The TKI revolution means that a 50-year-old CML patient diagnosed today can expect near-normal life expectancy — a dramatic contrast with the same diagnosis 25 years ago. A proportion of patients who achieve sustained deep molecular remission will be candidates for TKI discontinuation — an appealing goal for middle-aged patients who prefer a finite treatment course.
CLL begins to appear in this age group, though it is more common in older adults. Middle-aged CLL patients often face decisions about watchful waiting with the knowledge that they have a longer potential lifespan ahead, making the choice of treatment — and the durability of response — particularly important.
Leukemia Risk in Older Adults (Ages 60 and Beyond)
Older adults carry the highest absolute risk of leukemia, and the diseases most prevalent in this age group — AML, CLL, and CMML — are among the most challenging to treat because of the physiological constraints imposed by age and comorbidities.
AML in older adults (over 65) has historically been associated with very poor outcomes — 5-year survival below 10–15%. Two factors explain this: (1) the biology of older-adult AML is less favorable (higher rates of adverse cytogenetics, more therapy-related and secondary AML), and (2) older patients cannot safely receive the most intensive treatment regimens. The approval of azacitidine + venetoclax for previously untreated AML in patients who are not candidates for intensive chemotherapy — based on the VIALE-A trial — represents a major improvement for this population, achieving response rates of 65–70% and a meaningful survival advantage over standard low-intensity approaches.
CLL is primarily a disease of older adults. The median age at diagnosis (72 years) means that most CLL patients are already in this age group. Many will have multiple comorbidities that influence both treatment choice and the management of treatment complications. BTK inhibitors (particularly acalabrutinib and zanubrutinib) offer excellent tolerability profiles for older patients, including those who cannot tolerate chemoimmunotherapy.
CMML, with its median diagnosis age of 73, is almost exclusively a disease of older adults. Treatment decisions in this group are heavily influenced by performance status, comorbidities, and goals of care — making interdisciplinary discussions and careful assessment of patient preferences essential.
Environmental and Lifestyle Risk Factors
While the majority of leukemia cases arise without identifiable environmental causes, several risk factors have been established:
- Ionizing radiation: High-dose radiation exposure (atomic bomb survivors, therapeutic radiation for prior cancer) substantially increases leukemia risk, particularly AML and CML. Diagnostic medical radiation (X-rays, CT scans) contributes negligible risk at modern doses.
- Benzene: The most well-established occupational leukemogen. Benzene is a component of tobacco smoke, gasoline, and industrial solvents. Occupational benzene exposure (in rubber, shoe, and petroleum industries) increases AML and CLL risk.
- Tobacco smoking: Increases AML risk by approximately 1.5–2x. Tobacco smoke contains benzene and other leukemogens that are inhaled and distributed systemically.
- Prior chemotherapy: Alkylating agents (cyclophosphamide, melphalan) and topoisomerase II inhibitors (etoposide, doxorubicin) both increase secondary AML risk. Alkylator-related AML typically occurs 5–10 years after exposure; topoisomerase inhibitor-related AML occurs 2–3 years post-exposure and often carries specific translocations (11q23, 21q22).
- Formaldehyde: Classified as a human leukemogen by the International Agency for Research on Cancer (IARC); relevant for occupational exposures in anatomists, embalmers, and certain manufacturing workers.
- Pesticides and herbicides: Some epidemiological associations exist, though causality is less clearly established than for benzene or radiation.
Genetic Risk Factors
As discussed in our guide to the genetics of leukemia, several inherited conditions substantially increase leukemia risk:
- Down syndrome (trisomy 21) — 10–20x increased ALL risk; 500x increased infant AML risk
- Li-Fraumeni syndrome (TP53) — very high multiple cancer risk including AML
- Fanconi anemia — very high AML risk in childhood
- RUNX1 familial platelet disorder — ~35% lifetime AML risk
- GATA2 deficiency — high MDS/AML risk
- DDX41 germline mutation — MDS/AML in adults, particularly those over 50
Family history alone (without a known specific gene mutation) also confers modest risk. First-degree relatives of CLL patients have approximately a 3–7x increased risk of CLL. First-degree relatives of AML patients have a modest increased risk, largely driven by shared germline predisposition variants.
Reducing Leukemia Risk
Most leukemia is not preventable. However, modifiable risk factors can be addressed:
- Quit smoking — eliminating tobacco exposure reduces benzene and other leukemogen exposure
- Minimize occupational benzene exposure — proper workplace protections (ventilation, PPE) and occupational monitoring
- Use radiation therapy judiciously — where alternatives are available for treating prior cancers, discuss relative risks and benefits with your oncologist
- For individuals with known predisposing genetic conditions — engage with specialized leukemia surveillance programs at cancer centers with expertise in hereditary hematologic malignancy
Routine blood count screening for leukemia in the general population is not currently recommended. However, periodic CBC in individuals with known risk factors (prior chemotherapy, significant radiation exposure, known hereditary syndrome) is clinically appropriate and often practiced.
Patient Considerations
A leukemia diagnosis at any age is life-altering. Age-specific considerations — treatment intensity, fertility preservation, long-term medication adherence, survivorship monitoring — all reflect the life stage of the patient. Young adults should discuss fertility preservation before starting any potentially gonadotoxic therapy. Middle-aged patients should discuss the trade-off between treatment intensity and quality of life. Older adults should have explicit conversations about goals of care and whether the most intensive treatments align with their values and functional goals. For all ages, clinical trial participation is worth discussing — trials are not just for patients without treatment options; they often represent access to the best current care.
Caregiver Guidance
The caregiver experience differs significantly by patient age. Parents of children with leukemia navigate a pediatric cancer care system. Spouses and partners of middle-aged patients manage the intersection of cancer treatment with career, family, and financial responsibilities. Adult children caring for elderly parents face decisions about treatment intensity, quality of life, and end-of-life planning. Each caregiver situation is unique, and all benefit from connecting with specialized social work support and peer support networks at the treating leukemia center.
When to Seek Medical Evaluation
The threshold for seeking medical evaluation for leukemia symptoms should be low at any age — particularly if early warning signs are present. For older adults who attribute fatigue, bruising, and frequent infections to normal aging — know that these symptoms always warrant a blood count check, not a dismissal as "just getting older." For parents who notice limping, pallor, or unusual bruising in their child — seek evaluation promptly.
🚨 Universal Leukemia Emergency Warning Signs
- Fever above 101°F at any age — in a patient with known or suspected leukemia, this is always an emergency
- Uncontrolled bleeding
- Sudden severe breathlessness
- Neurological changes (confusion, weakness, sudden severe headache)
💬 Questions to Ask About Leukemia Risk at Your Life Stage
- Given my age, which leukemia type is most likely based on my symptoms and blood count?
- Do I have any known risk factors (prior chemotherapy, radiation, family history) that change my risk profile?
- Should I have periodic blood count monitoring given my risk factors?
- If I am diagnosed, how does my age influence treatment options and expected outcomes?
- Are fertility preservation options appropriate for my situation?
- What is the recommended follow-up and survivorship care for my age group after treatment?
This content is for informational and educational purposes only. It is not a substitute for professional medical advice, diagnosis, or treatment. Always consult your physician or a qualified healthcare provider with any questions about a medical condition. Never disregard professional medical advice or delay seeking it because of information you have read on this website. Read our full disclaimer.
Frequently Asked Questions
Leukemia has two peaks: in children aged 2–5 (mostly ALL) and in adults over 65 (CLL, AML, and CML are more common in older adults).
Yes — risk of AML, CLL, and most leukemia types increases significantly with age, with median diagnosis age around 66.
Prior cancer treatment (chemo/radiation), high-dose radiation exposure, benzene exposure, and certain genetic disorders like Down syndrome.
