📋 Quick Summary
- Topic: CAR-T cell therapy, bispecific antibodies, checkpoint inhibitors, and how these treatments harness the immune system.
- Key Takeaway: Early recognition and medical consultation are critical for the best clinical outcomes.
- Remember: Always consult a qualified healthcare professional if you have concerns.
Understanding Immunotherapy for Leukemia
Selecting the right leukemia treatment requires understanding not just the available modalities but how they interact with the specific biology of the patient's disease. The full spectrum of leukemia treatment options ranges from conventional chemotherapy to precision-targeted molecular drugs to cutting-edge immunotherapy — each appropriate for different disease subtypes, stages, and patient profiles. No single approach works for every patient, which is why treatment planning is inherently individualized and requires expert hematology-oncology guidance.
The specific treatment discussed in this article fits into a broader therapeutic ecosystem. It is rarely used in isolation: chemotherapy for leukemia often precedes or accompanies other modalities, acute lymphoblastic leukemia may be layered on top of conventional regimens, and relapsed and refractory leukemia management may be used to consolidate remission in high-risk disease. Understanding how the pieces fit together gives patients the framework to have more informed conversations with their oncology team.
Treatment decisions also depend critically on accurate diagnosis. The specific how leukemia is diagnosed — identified through a comprehensive workup including bone marrow biopsy, flow cytometry, and molecular genetic testing — dictates which therapies are likely to be effective. Patients whose disease carries specific molecular markers may qualify for targeted approaches that produce superior outcomes compared to standard chemotherapy alone. Additionally, clinical trials offer access to emerging therapies not yet widely available, and are worth discussing with your oncologist.
Pathophysiology and Clinical Significance
At the cellular level, leukemia cells (blasts in acute variants) lack the functional maturity of normal blood cells. They cannot effectively fight infections, transport oxygen, or assist in hemostasis. This produces the three-cytopenia triad — anemia, thrombocytopenia, and neutropenia — that underlies most leukemia symptoms. The article on leukemia treatment options explains how each subtype disrupts this balance differently.
- Erythropoiesis Suppression: Reduced red cell production leads to chemotherapy for leukemia, exertional breathlessness, pallor, and in severe cases, cardiovascular strain.
- Thrombocytopenia: Platelet counts fall, impairing hemostasis. Patients experience easy bruising, nosebleeds, bleeding gums, and prolonged bleeding from minor cuts — symptoms covered in detail in our article on acute lymphoblastic leukemia.
- Neutropenia: Functional white blood cell counts drop, creating severe immune compromise — explaining why relapsed and refractory leukemia management.
These three cytopenias account for most of the early complications of leukemia, and their severity correlates with disease stage and subtype. For a comprehensive overview of infections and immune health in leukemia, including the blood count patterns that reveal these cytopenias, see our full Diagnosis section.
Diagnostic Approach
When leukemia is suspected — typically triggered by early leukemia symptoms or an abnormal routine blood test — the workup follows a systematic process. It begins with a Complete Blood Count (CBC) with differential, progresses to a peripheral blood smear, and culminates in a bone marrow aspiration and biopsy for definitive characterization.
Molecular and cytogenetic analysis of marrow cells identifies the specific subtype and any targetable mutations — findings that directly determine which leukemia treatment options are most appropriate. For a detailed walkthrough of each diagnostic step, including what to expect and how to interpret results, see our guides on blood tests in leukemia diagnosis and understanding your leukemia test results.
Treatment Considerations
Treatment for leukemia is always individualized — determined by subtype, molecular risk category, patient age, and overall health. For acute leukemias, intensive induction how leukemia is diagnosed is typically the first step, aiming to rapidly clear leukemia cells and achieve remission. This may be followed by targeted therapy if molecular targets are identified, or by stem cell transplantation in high-risk disease.
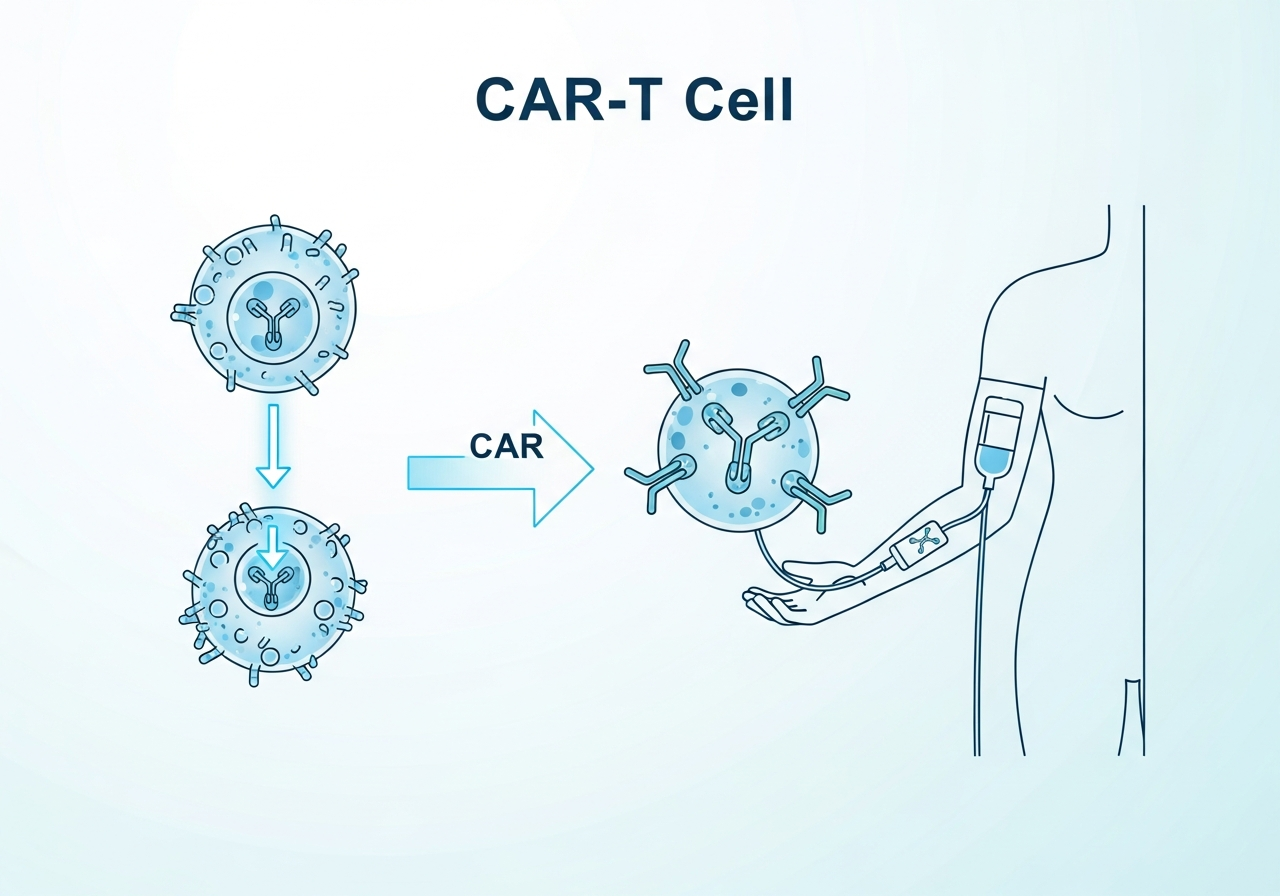
For chronic leukemias, the spectrum of treatment is broader: some patients undergo watchful waiting for years, while others begin oral targeted drugs immediately. Immunotherapy — including bispecific antibodies and CAR-T cell therapy — has emerged as a powerful option for relapsed or refractory cases. Patients are encouraged to ask about clinical trials, which often provide access to therapies not yet standard of care.
🚨 When to Seek Immediate Medical Attention
Contact a healthcare provider promptly or go to the nearest emergency room if you or a loved one experience:
- Severe shortness of breath at rest or with minimal activity
- Uncontrollable bleeding that does not stop with pressure
- Sudden confusion, severe dizziness, or loss of consciousness
- High fever (above 101°F / 38.3°C) that does not respond to medication
- Extreme, sudden-onset fatigue accompanied by chest pain
💬 Questions to Ask Your Healthcare Team
- How does this specific symptom or finding relate to my diagnosis?
- What diagnostic tests will you use to monitor my progress?
- How will my treatment plan address this particular aspect of my condition?
- Are there clinical trials relevant to my specific leukemia subtype?
- What should I watch for at home that would require urgent medical attention?
Related Leukemia Guides
This content is for informational and educational purposes only. It is not a substitute for professional medical advice, diagnosis, or treatment. Always consult your physician or a qualified healthcare provider with any questions about a medical condition. Never disregard professional medical advice or delay seeking it because of information you have read on this website. Read our full disclaimer.
Frequently Asked Questions
A treatment where a patient's own T-cells are extracted, genetically engineered to recognize leukemia cells, and reinfused to attack the cancer.
Currently FDA-approved primarily for relapsed/refractory ALL and certain lymphomas; research is expanding its use in other blood cancers.
Cytokine Release Syndrome (CRS), causing high fever and dangerous blood pressure drops, and neurological toxicity (ICANS) are the most serious risks.