📋 Quick Summary
- Topic: What clinical night sweats look like, why the immune response triggers them, and when to seek evaluation.
- Key Takeaway: Early recognition and medical consultation are critical for the best clinical outcomes.
- Remember: Always consult a qualified healthcare professional if you have concerns.
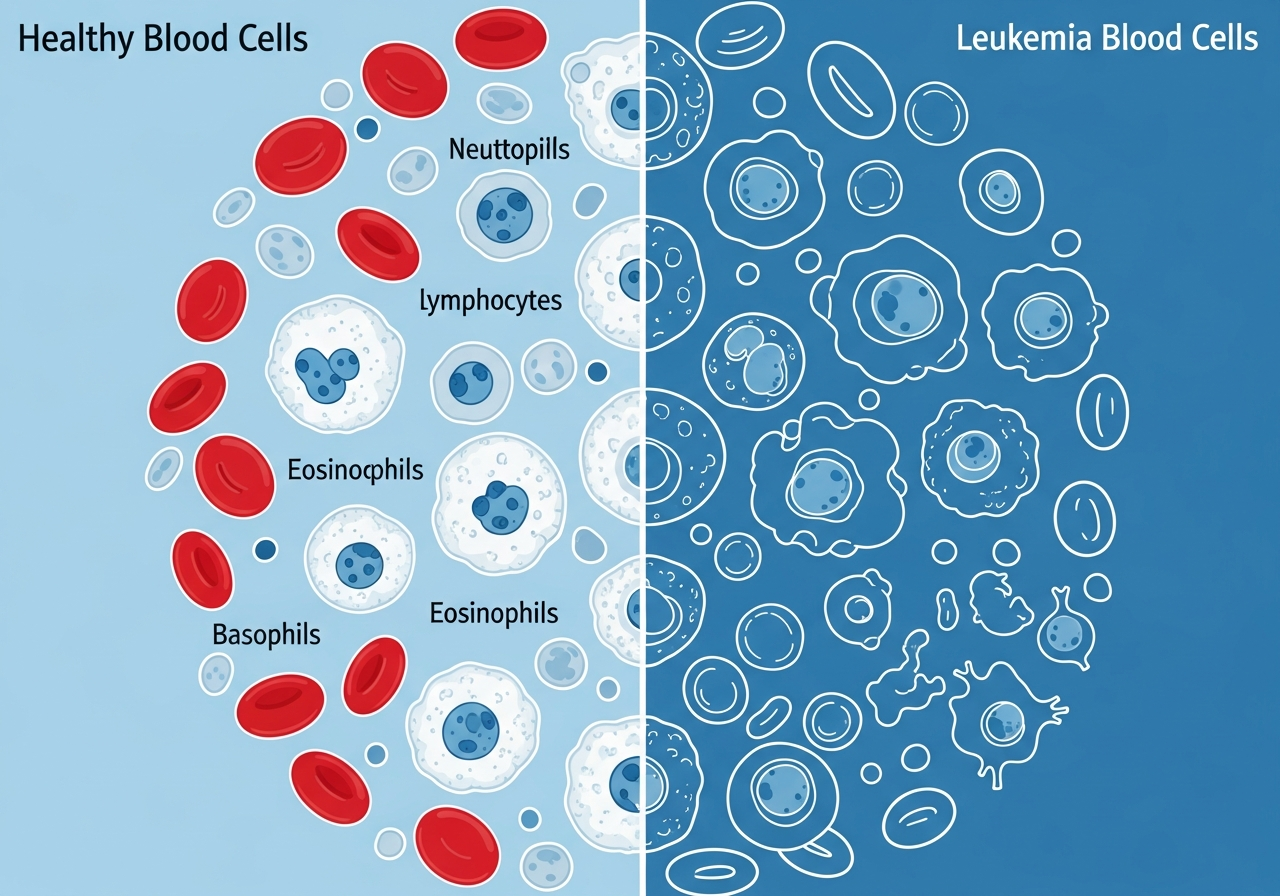
Night Sweats and Leukemia: Clinical Overview
Night sweats are among the most recognizable early warning signs of several blood cancers, including leukemia. While sweating during sleep is common and usually benign — caused by warm bedroom temperatures, heavy bedding, hormonal changes, or mild infections — clinical night sweats are qualitatively different: they are drenching, recurrent, unexplained by ambient temperature, and frequently severe enough to soak nightclothes or require changing bed sheets.
In oncology, drenching night sweats are part of what are called "B symptoms" — a cluster of constitutional symptoms that include fever and unexplained weight loss and that carry prognostic significance in lymphocytic malignancies. Their presence often indicates a more aggressive or advanced disease state and is taken seriously in staging and treatment planning for CLL, ALL, and lymphomas.
Patients who experience recurrent drenching night sweats — particularly alongside unexplained fatigue, lymph node swelling, or unintentional weight loss — should seek medical evaluation. A complete blood count is the appropriate first step.
Why Leukemia Causes Night Sweats: The Immunological Mechanism
The pathophysiology of leukemia-associated night sweats involves the immune system's response to the presence of abnormal leukemia cells in the body. This response is mediated by cytokines — soluble inflammatory signaling proteins that coordinate immune activity. In leukemia, the body recognizes that something is wrong and mounts an ongoing, low-grade inflammatory response. Key cytokines involved include:
- Interleukin-1 (IL-1): A potent pyrogen (fever-inducer) that also stimulates the hypothalamus — the brain's temperature-regulation center — to raise the body's set-point temperature. At night, as the body attempts to shed excess heat, sweating occurs.
- Tumor Necrosis Factor-alpha (TNF-α): Contributes to the systemic inflammatory state that drives both fever and sweating. TNF-α also suppresses appetite and contributes to cancer cachexia (weight loss).
- Interleukin-6 (IL-6): Elevates core body temperature and is found in elevated concentrations in the blood of many leukemia patients.
The result is a disrupted circadian rhythm of body temperature. Normally, body temperature drops at night, promoting sleep. In leukemia, cytokine-driven elevations in core temperature disrupt this drop and trigger episodic sweating as the thermoregulatory system attempts to compensate. Because the stimulus (cytokines from leukemia cells) is ongoing, the sweating episodes recur nightly until the underlying disease is treated.
Clinical Presentation of Leukemia-Associated Night Sweats
Clinically significant night sweats in leukemia share the following characteristics:
- Severity: Drenching — nightclothes or sheets are visibly wet. Mild dampness is not clinically significant.
- Frequency: Occurring on multiple nights per week rather than occasionally.
- Independence from temperature: Occur even in a cool, well-ventilated room. Not explained by excessive bedding or warm pajamas.
- Association with other symptoms: Rarely isolated — typically accompanied by fatigue, low-grade fever, or weight loss.
- Timing: Usually occur in the early morning hours (2–4 AM), when cortisol levels are low and the immune response is most active.
Patients often describe waking to find their pillowcase, shirt, and sheets soaked despite the room not being unusually warm. Some describe the sensation of waking suddenly from what feels like a fever, even though measured temperature may be only mildly elevated at that moment.
B Symptoms: Clinical Significance in Leukemia
In hematologic malignancies, the term "B symptoms" refers to a specific triad of constitutional symptoms:
- Drenching night sweats
- Unexplained fever above 38°C (100.4°F)
- Unexplained weight loss of more than 10% of body weight in the preceding 6 months
B symptoms are incorporated into the staging systems for Hodgkin and non-Hodgkin lymphoma, and they are recognized as prognostically significant in CLL (where they indicate more advanced or aggressive disease) and in ALL. Patients with B symptoms are generally considered to have a higher disease burden and are often started on treatment sooner. The presence of even two of the three B symptoms in a patient with an otherwise unexplained illness substantially raises the clinical suspicion for a lymphoproliferative or hematologic malignancy.
Other Causes of Night Sweats to Rule Out
Night sweats are a non-specific symptom with many causes. A thorough differential diagnosis is essential before attributing them to leukemia:
| Cause | Distinguishing Features |
|---|---|
| Menopause / perimenopause | Age-appropriate; hot flashes during day; no weight loss or lymphadenopathy |
| Infection (TB, HIV, endocarditis) | Exposure history; positive cultures or serologies; chest X-ray findings |
| Medications | Timing correlates with new medication; resolves with discontinuation |
| Hyperthyroidism | Elevated TSH/T4; tremor; weight loss with increased appetite |
| Anxiety / panic disorder | Normal CBC; no weight loss; psychological triggers identifiable |
| Alcohol use | Correlates directly with alcohol consumption; no lymphadenopathy |
| Leukemia / lymphoma | Abnormal CBC; lymphadenopathy; weight loss; fatigue; B-symptom cluster |
The presence of concurrent leukemia warning signs — particularly lymph node swelling, fatigue, pallor, or easy bruising — shifts the differential significantly toward a hematologic malignancy and mandates a complete blood count as a minimum workup.
Diagnostic Approach When Night Sweats Raise Concern
When a patient presents with recurrent drenching night sweats without an obvious benign explanation, the initial workup should include:
- Complete Blood Count (CBC) with differential: The cornerstone of leukemia evaluation. May reveal elevated or depressed white blood cell counts, anemia, or thrombocytopenia.
- Comprehensive metabolic panel: Assesses liver and kidney function; may show elevated LDH (lactate dehydrogenase) — a marker of cell turnover elevated in many leukemias.
- Thyroid function tests: Rules out hyperthyroidism as a cause.
- Infectious workup: Chest X-ray, tuberculosis testing (if indicated), and HIV serology.
- Peripheral blood smear: Microscopic examination of blood cells can reveal blast cells or atypical lymphocytes suggesting leukemia.
If the CBC is abnormal or the clinical picture is suspicious despite a normal initial CBC, urgent referral to a hematologist for consideration of bone marrow biopsy is appropriate. Understanding what all these tests mean is explained in our guide to interpreting leukemia test results.
How Treatment Resolves Night Sweats
In leukemia, night sweats are a consequence of the disease — they are not treated directly but rather resolve as the underlying malignancy is controlled. When chemotherapy, targeted therapy, or other treatments successfully reduce the leukemia cell burden, cytokine production falls and night sweats typically improve within weeks. In CLL treated with BTK inhibitors like ibrutinib or acalabrutinib, B symptoms often begin to resolve within the first few months of therapy as disease control is achieved.
During active treatment, night sweats may temporarily worsen due to treatment-related fever and inflammation (particularly during induction chemotherapy or after stem cell transplantation). In this context, clinical teams monitor closely for infections that can cause similar symptoms.
Prognostic Significance
The presence of night sweats as a B symptom is incorporated into staging systems and treatment planning. In CLL, for example, B symptoms (including night sweats) indicate a higher Rai or Binet stage and are often one of the triggers for initiating treatment in patients who would otherwise be observed. In ALL and AML, the constitutional symptoms of advanced disease — including night sweats — indicate a higher tumor burden that may correlate with more aggressive biology.
However, it is important for patients to understand that night sweats themselves do not determine prognosis — the specific leukemia type, subtype, and molecular characteristics are far more determinative. Many patients with significant night sweats achieve excellent outcomes with appropriate treatment.
Managing Night Sweats During Treatment
While definitive treatment addresses the root cause, several practical strategies help patients manage night sweats during the diagnostic period or while awaiting treatment response:
- Keep the bedroom cool (below 68°F / 20°C) and well-ventilated
- Use moisture-wicking or lightweight bedding and sleepwear
- Keep a change of nightclothes and a dry towel at the bedside
- Avoid alcohol and spicy foods in the evening, which can trigger or worsen sweating
- Stay well-hydrated — sweating at night leads to significant fluid loss that should be replaced
- Track the frequency and severity of episodes for your medical team
Caregiver Guidance
Night sweats profoundly disrupt the sleep of both the patient and their bed partner. Caregivers who share a sleeping space may wish to consider separate arrangements temporarily — not as a rejection but as a practical measure that protects both parties' sleep quality, which is essential during a difficult treatment period. Caregivers should note the frequency and severity of night sweat episodes to report to the medical team, as this provides valuable information about treatment response or disease activity.
When to Seek Medical Attention
Night sweats alone are rarely a medical emergency. However, prompt (non-emergency) medical evaluation is appropriate for:
- Drenching night sweats occurring more than twice per week without a clear benign explanation
- Night sweats occurring alongside unexplained weight loss, swollen lymph nodes, or persistent fatigue
- Night sweats in a patient with a known history of any hematologic malignancy — these may indicate disease progression
Emergency evaluation is warranted if night sweats are accompanied by high fever, rigors (uncontrolled shaking chills), rapid heart rate, and confusion — this combination may indicate sepsis in an immunocompromised patient.
🚨 When Night Sweats Require Emergency Care
- High fever (above 101°F) with chills and rapid heart rate — possible sepsis
- Confusion or disorientation alongside sweating and fever
- Known leukemia diagnosis with sudden worsening of night sweats and new symptoms
💬 Questions to Ask Your Doctor About Night Sweats
- Are my night sweats the "drenching" type that warrants a blood work evaluation?
- Should I be checked for infections like tuberculosis or HIV as possible causes?
- Do I have any other findings — lymph node swelling or abnormal blood counts — that suggest a blood cancer?
- What is the B-symptom significance of my night sweats in relation to my diagnosis?
- Will my night sweats improve once treatment starts, and how quickly?
- Are there any medications that can help with the sweats while we await treatment response?
This content is for informational and educational purposes only. It is not a substitute for professional medical advice, diagnosis, or treatment. Always consult your physician or a qualified healthcare provider with any questions about a medical condition. Never disregard professional medical advice or delay seeking it because of information you have read on this website. Read our full disclaimer.
Frequently Asked Questions
No — night sweats can be caused by menopause, anxiety, infections, or medications. Drenching night sweats that require changing bedclothes should be evaluated.
If you experience frequent, drenching night sweats accompanied by unexplained weight loss or fever, consult a healthcare provider promptly.
The body's immune response to leukemia cells releases inflammatory chemicals (cytokines) that disrupt temperature regulation, triggering sweating.
