📋 Quick Summary
- Topic: A guide to definitive warning signs of leukemia, differentiating red flags from everyday ailments.
- Key Takeaway: Early recognition and medical consultation are critical for the best clinical outcomes.
- Remember: Always consult a qualified healthcare professional if you have concerns.
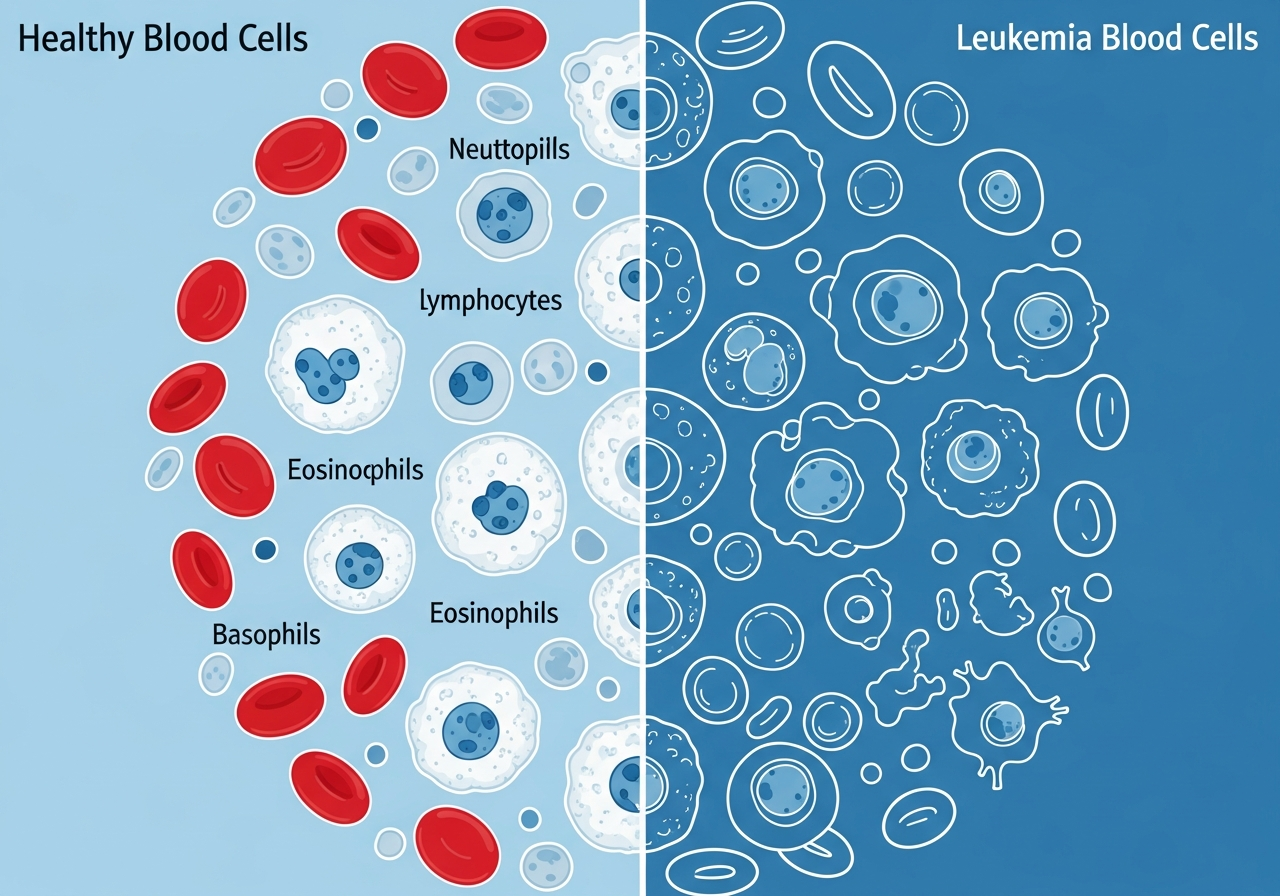
Understanding Leukemia Warning Signs
Leukemia warning signs are the clinical signals that distinguish a potentially serious blood disorder from common benign illness. While no single warning sign is specific to leukemia — each individual symptom can be caused by dozens of conditions — the combination of several warning signs occurring together, persisting despite treatment, or worsening over time is what clinicians and patients should recognize as a call to action.
Leukemia — which encompasses more than a dozen distinct subtypes spanning Acute Lymphoblastic Leukemia (ALL), Acute Myeloid Leukemia (AML), Chronic Lymphocytic Leukemia (CLL), and Chronic Myeloid Leukemia (CML) — shares a common biological mechanism: abnormal blood-forming cells proliferate in the bone marrow and crowd out healthy red blood cells, white blood cells, and platelets. The resulting cytopenias produce almost all of the classic warning signs described on this page.
Recognizing these warning signs is not just about individual awareness — it is a public health priority. Delayed diagnosis of acute leukemia, in particular, allows the disease to advance to a stage where treatment is more dangerous and outcomes are worse. Early symptom recognition is one of the most actionable tools available to patients and their families.
The Key Leukemia Warning Signs
The following warning signs, particularly when occurring in combination or persisting unexplained for more than two weeks, should prompt a prompt medical evaluation including a complete blood count:
1. Unexplained, Persistent Fatigue
Leukemia-related fatigue is the most common and often most debilitating warning sign. It arises primarily from anemia — the reduction in functional red blood cells caused by bone marrow failure. This is not the tiredness of a poor night's sleep; it is a bone-deep exhaustion that limits the ability to work, exercise, or complete daily tasks, and it does not improve with rest.
2. Frequent, Severe, or Slow-Resolving Infections
When leukemia cells displace healthy white blood cells, the body loses its primary defense against pathogens. Patients may suffer recurrent sinusitis, pneumonia, urinary tract infections, or mouth sores that either recur frequently or fail to resolve despite antibiotics. Immune compromise in leukemia is not merely an inconvenience — it is the leading cause of death in untreated and inadequately treated leukemia patients.
3. Easy Bruising and Abnormal Bleeding
When platelet production is suppressed, even trivial trauma produces disproportionate bruising. Blood clotting problems in leukemia range from frequent nosebleeds and bleeding gums to prolonged bleeding from cuts and, in severe cases, spontaneous bleeding into organs. Women may experience significantly heavier menstrual periods. Any unexplained bleeding tendency warrants a platelet count.
4. Painless, Firm, Enlarged Lymph Nodes
Swollen lymph nodes are a particularly common warning sign of lymphocytic leukemias (ALL and CLL). Unlike the tender, transient lymph nodes that swell during a bacterial or viral infection, leukemia-related lymphadenopathy is typically painless, firm, and persistent — lasting weeks or months without a clear infectious cause. Nodes in the neck, armpits, and groin are the most accessible to self-examination.
5. Unexplained Weight Loss
Losing 5% or more of body weight over six months without dietary change or increased physical activity is medically significant. In leukemia, unexplained weight loss occurs because rapidly dividing leukemia cells are metabolically demanding, consuming nutrients and energy that would otherwise maintain body mass. Additionally, enlarged spleen pressing on the stomach causes early satiety, reducing food intake.
6. Night Sweats
Drenching night sweats that require changing bedclothes or sheets are a recognized warning sign of several leukemia types and lymphomas. They arise from the immune system's inflammatory response to leukemia cells, including the release of cytokines (inflammatory signaling molecules) that disrupt the body's normal temperature regulation. Occasional mild sweating is normal, but repeated drenching episodes warrant evaluation.
7. Bone or Joint Pain
Less commonly recognized, bone pain is a warning sign — particularly in ALL. As leukemia cells expand within the bone marrow, they exert increasing pressure on the bone itself and on nerve endings in the periosteum (bone surface). This manifests as a deep aching pain in the long bones, ribs, sternum, or spine that may worsen at night.
8. Pallor and Skin Changes
Anemia produces visible pallor — particularly noticeable in the skin, lips, gums, and conjunctiva (the inner surface of the eyelids). Additionally, leukemia-specific skin changes may occur, including petechiae (tiny red pinpoint spots from microbleeds), large bruises from minor trauma, or — rarely — leukemia cutis (leukemia cell infiltration of the skin producing firm, discolored nodules).
9. Abdominal Fullness and Discomfort
When leukemia cells infiltrate the spleen and liver, these organs enlarge significantly. Patients feel abdominal discomfort or fullness — particularly in the upper left abdomen (from spleen enlargement) — and may experience early satiety: feeling full after eating only small amounts. In advanced cases, the enlarged spleen may be visible or palpable.
10. Shortness of Breath
When anemia is severe, the body cannot deliver adequate oxygen even at rest. Shortness of breath on minimal exertion — walking up stairs, talking, or mild activity — is a warning sign that anemia has reached a clinically significant level. In ALL, enlarged mediastinal (chest cavity) lymph nodes can also compress the airways, adding a mechanical component to breathing difficulty.
How Warning Signs Differ from Common Illness
The clinical challenge with leukemia warning signs is that each individual symptom has far more common, benign explanations. The table below outlines the key distinguishing features:
| Warning Sign | Common Benign Cause | Features Suggesting Leukemia |
|---|---|---|
| Fatigue | Poor sleep, stress, anemia from diet | Does not improve with rest; accompanied by pallor |
| Frequent infections | Seasonal viruses, poor hand hygiene | Unusual pathogens; slow resolution; multiple concurrent sites |
| Bruising | Trauma, aspirin use, aging | No trauma history; multiple large bruises; petechiae |
| Swollen lymph nodes | Viral or bacterial infection | Painless; firm; persists >2 weeks after infection resolves |
| Night sweats | Menopause, anxiety, alcohol | Drenching; requires bedding change; occurs with other B symptoms |
| Weight loss | Dietary change, increased activity | No intentional change; >5% loss in 6 months |
Warning Signs by Leukemia Type
Different leukemia types tend to produce different warning sign patterns:
- ALL (Acute Lymphoblastic Leukemia): Rapid onset over days to weeks; bone pain; lymphadenopathy; CNS involvement possible.
- AML (Acute Myeloid Leukemia): Rapid onset; severe cytopenias; bleeding particularly prominent; gingival (gum) infiltration in some subtypes.
- CLL (Chronic Lymphocytic Leukemia): Often asymptomatic; discovered on routine blood test; lymphadenopathy; fatigue in later stages; increased infection susceptibility.
- CML (Chronic Myeloid Leukemia): Often silent early; fatigue; spleen enlargement; left-side abdominal fullness; discovered incidentally.
The Diagnostic Pathway After Warning Signs
When warning signs prompt medical evaluation, the physician will typically order a complete blood count (CBC) with differential. Abnormal results — markedly elevated or depressed white blood cell counts, anemia, thrombocytopenia, or the presence of blast cells on peripheral smear — prompt urgent hematology referral. The definitive diagnosis is made by bone marrow biopsy, which allows full characterization of the leukemia type, subtype, and molecular features. For a guide to interpreting results, see our article on understanding leukemia test results.
Treatment Urgency Based on Warning Signs
Not all leukemia warning signs carry the same urgency. In acute leukemias, warning signs should prompt emergency evaluation — the disease can progress to life-threatening complications within days. In chronic leukemias, warning signs are important but typically allow time for scheduled appointments rather than emergency visits.
When leukemia is confirmed, treatment is selected based on type and molecular features. Options range from chemotherapy to oral targeted therapy, immunotherapy, and potentially stem cell transplantation. Enrollment in clinical trials is increasingly recommended for access to emerging therapies.
Prognosis Context
Leukemia prognosis is highly variable and depends primarily on the specific subtype, molecular features, patient age, and how promptly treatment begins. Childhood ALL has a cure rate exceeding 90% with modern therapy. CML has been transformed into a manageable chronic condition by tyrosine kinase inhibitors. AML remains the most challenging — particularly in older adults — though outcomes continue to improve with targeted agents. For all types, acting on warning signs earlier translates to a broader range of treatment options and generally better outcomes.
Patient Considerations
Patients who recognize any of these warning signs in themselves should document them — timing of onset, frequency, severity, and any associated factors. This information is invaluable at the first medical appointment. Patients should not self-dismiss symptoms with reassuring explanations (fatigue from overwork, bruising from gym activity) if the pattern is persistent and unexplained.
It is also important for patients to advocate clearly for a CBC when they present with multiple warning signs. While most cases will have benign explanations, the cost and risk of a blood test are negligible, and the information it provides is enormous. Patients who have a known family history of hematologic malignancy or who carry known leukemia risk factors (prior chemotherapy, radiation, benzene exposure) have an even stronger basis for proactive screening.
Caregiver Guidance
Caregivers, family members, and parents are uniquely positioned to notice warning signs that the patient may dismiss or not report. Visible signs — pallor, petechiae, unusual bruising, lymph node swelling — are often noticed by others before the patient themselves. Children with bone pain may not verbalize it clearly, instead becoming irritable, refusing to walk, or seeming generally unwell without a clear explanation. Caregivers who are alert to these patterns and who communicate their observations clearly to healthcare providers may shorten the diagnostic pathway significantly.
When to Seek Urgent Medical Care
Several warning signs require emergency evaluation rather than a routine medical appointment:
- Fever above 101°F (38.3°C) that does not respond to over-the-counter medication, especially with chills or rigors — this may indicate sepsis in an immunocompromised patient
- Any bleeding that does not stop within 10–15 minutes of sustained direct pressure
- Severe, sudden-onset shortness of breath at rest
- Sudden confusion, weakness, numbness, or loss of consciousness — these may indicate CNS involvement or intracranial bleeding
- Rapidly spreading petechiae or purpura (purple skin discoloration from bleeding under the skin)
🚨 Seek Emergency Care Immediately For:
- Unresponsive fever with chills in anyone with a known low white blood cell count
- Bleeding that will not stop with sustained pressure
- Sudden confusion, stroke-like symptoms
- Severe breathlessness at rest
💬 Questions to Ask Your Doctor
- Which of my warning signs are most concerning given my age and health history?
- Should I have a complete blood count today, and what do my results mean?
- At what point would you refer me to a hematologist?
- Are any of my warning signs consistent with a specific leukemia type?
- How quickly does this type of leukemia typically progress if left untreated?
- What signs at home should cause me to go directly to the emergency room?
This content is for informational and educational purposes only. It is not a substitute for professional medical advice, diagnosis, or treatment. Always consult your physician or a qualified healthcare provider with any questions about a medical condition. Never disregard professional medical advice or delay seeking it because of information you have read on this website. Read our full disclaimer.
Frequently Asked Questions
Persistent fatigue, frequent infections, unexplained weight loss, enlarged lymph nodes, and abdominal fullness are key warning signs.
No — fever is a symptom of many conditions. Recurrent, unexplained fever without obvious cause warrants a medical evaluation.
Uncontrollable bleeding, severe shortness of breath, sudden confusion, or extreme weakness require immediate emergency attention.
