📋 Quick Summary
- Topic: Anemia-driven breathlessness, organ involvement, and when breathing difficulty becomes a medical emergency.
- Key Takeaway: Early recognition and medical consultation are critical for the best clinical outcomes.
- Remember: Always consult a qualified healthcare professional if you have concerns.
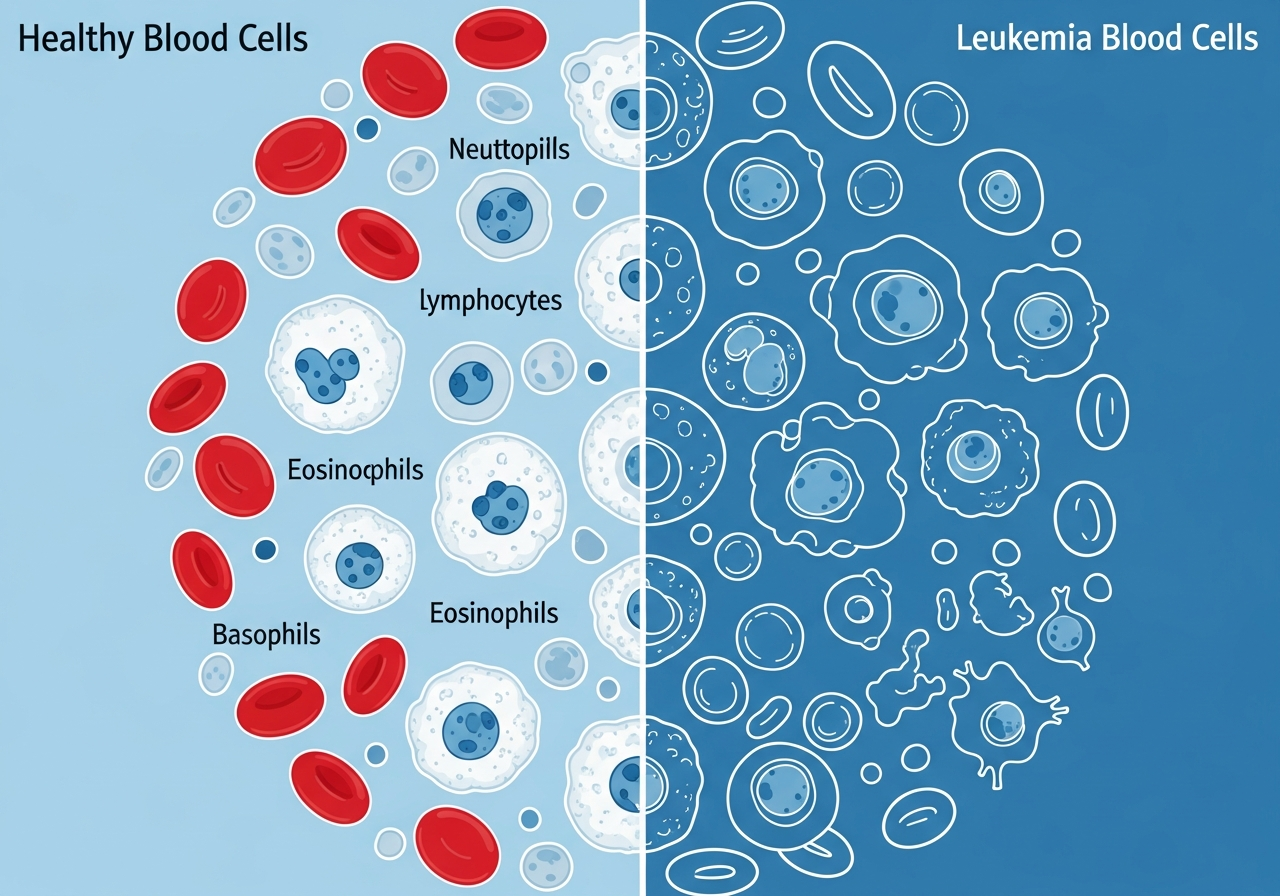
Shortness of Breath in Leukemia: An Important Warning Sign
Shortness of breath — the subjective sensation of breathing difficulty or inadequate air — is a significant symptom in leukemia that is often underappreciated compared to more visible signs like bruising or lymph node swelling. In leukemia, breathlessness arises primarily from severe anemia (inadequate oxygen-carrying capacity) and, in some cases, from direct physical compression of airways or from lung complications of the disease or its treatment. All breathlessness symptoms, when they occur alongside other signs, should prompt a visit to our complete leukemia symptoms guide.
Understanding why leukemia causes breathing difficulty — and crucially, when that difficulty constitutes a medical emergency — is essential knowledge for patients, families, and anyone involved in the care of a leukemia patient. Breathlessness in a leukemia patient is never entirely benign and always warrants assessment. The specific underlying cause depends partly on which type of leukemia is present — T-cell ALL, for example, is especially associated with mediastinal masses that compress the airways, while AML may cause breathlessness through severe anemia or leukostasis at very high blast counts.
Breathlessness frequently accompanies other leukemia warning signs: profound fatigue, pallor, rapid heart rate, and difficulty with activities that previously required little effort. When these symptoms cluster, the clinical team must act promptly — starting with a complete blood count to measure hemoglobin and rule out extreme leukocytosis, and progressing to a bone marrow evaluation if leukemia is suspected.
The Main Causes of Breathlessness in Leukemia
1. Anemia-Driven Breathlessness (Most Common)
The most common cause of shortness of breath in leukemia is severe anemia. Red blood cells carry hemoglobin, which binds and transports oxygen from the lungs to every cell in the body. When leukemia cells displace normal bone marrow precursors, red blood cell production (erythropoiesis) is suppressed. The resulting anemia means that each breath delivers a reduced oxygen load — a problem compounded by the body's increased oxygen demands from fever, infection, or rapid cancer cell metabolism.
When hemoglobin falls below approximately 8 g/dL (normal is 12–17 g/dL), most patients begin experiencing dyspnea (shortness of breath) on exertion — walking, climbing stairs, or other physical activity. At very low levels (below 6–7 g/dL), breathlessness may occur even at rest. The body compensates by increasing heart rate (tachycardia) and respiratory rate, which can cause palpitations, dizziness, and chest discomfort in addition to breathlessness.
2. Leukostasis (In Very High White Blood Cell Counts)
In some acute leukemias — particularly AML and ALL — white blood cell counts can become extremely elevated (hyperleukocytosis, generally defined as WBC count above 100,000 cells/μL). Leukemia blasts are larger and less deformable than normal red blood cells, and at very high concentrations they can physically obstruct small blood vessels in the lungs (pulmonary leukostasis), causing breathlessness, hypoxia (low blood oxygen), and potentially respiratory failure. This is a hematologic emergency requiring urgent treatment.
3. Mediastinal Mass (Especially in T-cell ALL)
In T-cell Acute Lymphoblastic Leukemia, leukemia cells can accumulate in the thymus and mediastinal lymph nodes — the structures in the chest cavity between the lungs. This produces a mediastinal mass that can compress the trachea (windpipe) and/or the superior vena cava (the major vein returning blood from the upper body to the heart). Airway compression causes shortness of breath, wheezing, and a characteristic positional worsening — patients feel more breathless when lying flat and less breathless when sitting upright. This is a medical emergency that can rapidly progress to airway obstruction.
4. Pulmonary Infections
Because leukemia suppresses immunity, the lungs are vulnerable to severe infections — including bacterial pneumonia, fungal pneumonia (aspergillosis, Pneumocystis jirovecii pneumonia), and viral pneumonitis. These infections cause breathlessness through inflammation and fluid accumulation in the lung tissue. In immunocompromised leukemia patients, pulmonary infections can deteriorate very rapidly and must be treated aggressively.
5. Treatment-Related Lung Complications
Several leukemia treatments can affect the lungs. High-dose chemotherapy prior to stem cell transplantation can cause inflammation of the lung lining. Graft-versus-Host Disease (GVHD) after allogeneic transplantation can affect the lungs (bronchiolitis obliterans). CAR-T cell therapy can produce cytokine release syndrome with significant respiratory involvement. All of these require immediate clinical assessment when breathing difficulty develops during or after treatment.
Clinical Presentation of Breathlessness in Leukemia
The breathlessness experienced by leukemia patients varies by cause and severity:
- Exertional dyspnea: Initially occurs only with moderate physical effort — climbing stairs, walking briskly. This is the earliest presentation of anemia-related breathlessness.
- Dyspnea on minimal exertion: As anemia worsens, even light activities — slow walking, speaking, bathing — become breathless. This indicates more severe anemia or pulmonary involvement.
- Resting dyspnea: Shortness of breath at rest is a serious finding indicating very low hemoglobin, significant pulmonary complications, or leukostasis. This requires urgent evaluation.
- Orthopnea: Breathlessness that worsens when lying flat — a classic sign of mediastinal mass in T-cell ALL, or of cardiac involvement. Patients instinctively sleep sitting up or with multiple pillows.
- Stridor: A high-pitched, audible wheezing or squeaking with each breath — indicates significant airway narrowing, potentially from mediastinal mass or lymph node compression. This is an emergency.
| Cause | Key Features | Urgency |
|---|---|---|
| Anemia (low hemoglobin) | Exertional; pallor; fatigue; tachycardia | Urgent if at rest; routine if mild exertional |
| Leukostasis (very high WBC) | Extremely high WBC count; acute onset; confusion | Emergency |
| Mediastinal mass | Worsens lying flat; stridor; SVC syndrome | Emergency |
| Pulmonary infection | Fever; cough; new chest findings on X-ray | Urgent to emergency |
| Treatment-related (GVHD, CAR-T) | Timing correlates with treatment; systemic symptoms | Urgent |
Mediastinal Mass in T-Cell ALL: A Critical Presentation
T-cell ALL accounts for approximately 15–25% of adult ALL cases and a smaller proportion of pediatric cases. It has a distinctive clinical presentation: up to 70% of patients with T-cell ALL develop a mediastinal mass from thymic and mediastinal lymph node involvement at the time of diagnosis. This is one of the most medically urgent presentations in all of hematologic oncology.
The mediastinal mass can compress the trachea, the superior vena cava, and adjacent structures. The resulting symptoms include shortness of breath (especially lying flat), facial or arm swelling (from SVC compression), and hoarseness. If airway compromise becomes severe, the patient may be unable to maintain an adequate airway without mechanical support. For this reason, any young patient presenting with shortness of breath, facial swelling, and an anterior chest mass must be evaluated as a potential hematologic emergency.
Diagnostic Evaluation of Breathlessness in a Leukemia Patient
When a leukemia patient (or a newly presenting patient with suspected leukemia) develops breathlessness, the clinical workup must move quickly:
- CBC and hemoglobin: The first step — determines whether anemia is the cause and its severity. A complete blood count also reveals the white blood cell count, identifying possible hyperleukocytosis.
- Pulse oximetry: Measures blood oxygen saturation. Values below 92% indicate significant hypoxia requiring immediate intervention.
- Chest X-ray: May reveal mediastinal widening (from a mediastinal mass), pulmonary infiltrates (infection), or pleural effusion.
- CT chest: More detailed than X-ray; characterizes mediastinal mass extent, airway compression degree, and pulmonary pathology.
- Arterial blood gas: Quantifies oxygen and carbon dioxide levels in the blood; guides decisions about supplemental oxygen and ventilatory support.
Treatment and Management of Breathlessness
Treatment targets the underlying cause:
- Anemia-related breathlessness: Red blood cell transfusions to restore hemoglobin to a safe level (typically above 8 g/dL). Effective leukemia treatment addresses the root cause by restoring normal bone marrow function.
- Leukostasis: Emergency leukapheresis (physical removal of excess white blood cells from the blood) and/or urgent cytoreductive chemotherapy.
- Mediastinal mass: Prompt initiation of ALL treatment — corticosteroids and chemotherapy rapidly reduce lymphoblast mass. General anesthesia carries extreme risk in these patients, so invasive procedures are avoided until the mass has reduced.
- Pulmonary infection: Broad-spectrum antibiotics for bacterial infection; antifungals for fungal pneumonia; antivirals as appropriate. Bronchoscopy may be needed for precise pathogen identification.
Prognosis and Recovery of Breathing
In most cases of leukemia-related breathlessness, the symptom resolves as treatment achieves disease control. Anemia-related breathlessness improves reliably with transfusion and with effective leukemia treatment that allows marrow recovery. Mediastinal mass breathlessness responds dramatically to initial chemotherapy in most T-cell ALL patients. Pulmonary infections, if caught early, can typically be controlled with appropriate antimicrobial therapy in the context of overall leukemia management.
Patient Self-Monitoring for Breathing Changes
Leukemia patients should be taught to monitor for worsening breathlessness and to communicate changes promptly. Practical self-monitoring guidance includes:
- Know your baseline: note the activity level at which breathlessness begins and communicate any reduction in that threshold to your medical team
- Avoid activities that significantly worsen breathlessness until the cause is investigated
- A home pulse oximeter (available inexpensively) can provide an objective measure of oxygen saturation; readings below 92% at rest warrant medical contact
- Sleep in a position that is most comfortable — patients with mediastinal mass often find a semi-upright position less breathless
Caregiver Guidance
Caregivers should observe breathing pattern and rate at rest and with activity. Any noticeable increase in respiratory rate at rest (more than 20 breaths per minute), use of accessory muscles (neck and shoulder muscles visible while breathing), or audible stridor are emergency signs. Caregivers should also watch for cyanosis — a bluish tint to the lips, fingernails, or skin — which indicates severely reduced blood oxygen and requires immediate emergency response. Know the route to the nearest emergency room in advance.
When to Seek Emergency Care
The following situations require immediate emergency evaluation — do not wait for the next clinic appointment:
- Breathlessness at rest that is new or rapidly worsening
- Oxygen saturation below 92% on a home oximeter
- Bluish lips, fingernails, or skin
- Stridor — audible high-pitched noise with each breath
- Breathlessness that is significantly worse lying flat
- Breathlessness accompanied by chest pain, rapid heart rate, or confusion
- Any breathing difficulty in a known leukemia patient that is new or markedly worse than baseline
🚨 Call 911 or Go to the Emergency Room Immediately For:
- Breathlessness at rest or with talking
- Oxygen saturation below 92%
- Bluish discoloration of lips or fingernails
- Audible wheezing or stridor with each breath
- Chest pain or confusion alongside breathlessness
💬 Questions to Ask Your Healthcare Team
- Is my hemoglobin level contributing to my breathlessness, and do I need a transfusion?
- Does my imaging show any mediastinal mass or lung involvement?
- What oxygen saturation level should prompt me to call or come in?
- Should I have a home pulse oximeter?
- Are there any activities I should avoid because of my current breathing capacity?
- How quickly do you expect my breathing to improve once treatment begins?
This content is for informational and educational purposes only. It is not a substitute for professional medical advice, diagnosis, or treatment. Always consult your physician or a qualified healthcare provider with any questions about a medical condition. Never disregard professional medical advice or delay seeking it because of information you have read on this website. Read our full disclaimer.
Frequently Asked Questions
Leukemia crowds out healthy red blood cells, causing anemia. With fewer cells to carry oxygen, the body struggles to meet its needs.
If it occurs suddenly, at rest, or with chest pain, dizziness, or a bluish tint to the lips, seek emergency care immediately.
Blood transfusions to restore red blood cell counts, supplemental oxygen, and targeted leukemia therapies all help.
