📋 Quick Summary
- Topic: What ALL is, who it affects, symptoms, diagnosis, treatment, and prognosis — including pediatric and adult differences.
- Key Takeaway: Early recognition and medical consultation are critical for the best clinical outcomes.
- Remember: Always consult a qualified healthcare professional if you have concerns.
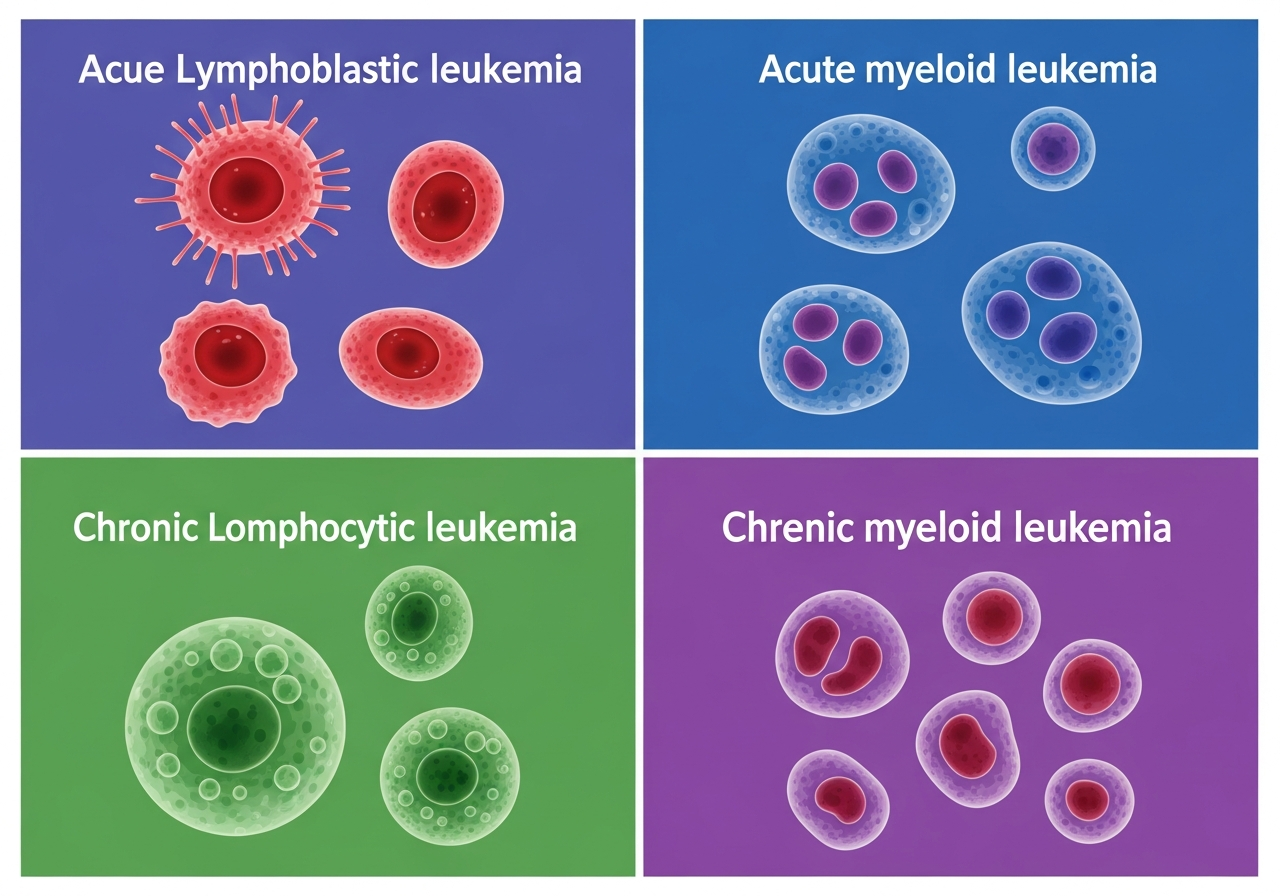
Acute Lymphoblastic Leukemia (ALL): A Complete Guide
Acute Lymphoblastic Leukemia (ALL) is a rapidly progressing cancer of lymphoid progenitor cells — the immature cells that would normally mature into B lymphocytes, T lymphocytes, or NK cells. In ALL, these progenitor cells undergo malignant transformation and proliferate uncontrollably in the bone marrow, rapidly crowding out normal hematopoietic cells and spilling into the bloodstream and lymphatic system.
ALL is the most common cancer in children, accounting for approximately 25–30% of all pediatric cancers and 75–80% of childhood leukemia diagnoses. It also occurs in adults, though with a different molecular landscape and less favorable prognosis. The peak incidence in children occurs between ages 2 and 5. In adults, incidence rises again in the elderly (age 65+).
Modern treatment of childhood ALL is one of oncology's great successes — cure rates now exceed 90% at specialized pediatric cancer centers, achieved through decades of systematic refinement of multi-agent chemotherapy protocols. Adult ALL remains more challenging, but outcomes are improving rapidly with targeted therapies and immunotherapy.
The Biology of ALL
ALL arises from the malignant transformation of a lymphoid progenitor cell at various stages of normal B-cell or T-cell development. The specific stage of arrest and the associated genetic/chromosomal abnormalities determine the ALL subtype and its clinical behavior.
The fundamental defects in ALL cells include:
- Blocked differentiation: The leukemia cells are "frozen" at an immature stage of development and cannot mature into functional lymphocytes.
- Impaired apoptosis: Normal mechanisms of programmed cell death are bypassed, allowing leukemia cells to accumulate.
- Abnormal self-renewal: Cancer stem cells continue to generate new leukemia cells indefinitely.
- Marrow infiltration: As ALL blasts accumulate, they physically and biochemically suppress production of red blood cells, platelets, and normal white blood cells — producing the cytopenias that generate most ALL symptoms.
ALL Subtypes: B-Cell, T-Cell, and Molecular Classification
B-Cell ALL (B-ALL)
B-ALL accounts for approximately 85% of ALL cases and arises from B-lymphocyte precursors. It is further subclassified by immunophenotype and molecular/cytogenetic features:
- Hyperdiploidy (more than 50 chromosomes): The most common favorable cytogenetic finding; excellent response to methotrexate-based therapy; cure rates exceed 90% in children.
- ETV6-RUNX1 (TEL-AML1) fusion: Present in ~25% of childhood B-ALL; favorable prognosis; good response to standard therapy.
- BCR-ABL1 (Philadelphia chromosome, Ph+) ALL: Present in ~3–5% of childhood ALL and ~25–30% of adult ALL; historically high-risk; now treated with TKIs (dasatinib, ponatinib) alongside chemotherapy with dramatically improved outcomes.
- Ph-like (BCR-ABL1-like) ALL: A high-risk group with gene expression patterns similar to Ph+ ALL but lacking BCR-ABL1; many have other targetable kinase fusions; poor outcome with standard therapy.
- iAMP21 (intrachromosomal amplification of chromosome 21): High-risk; requires intensive therapy.
- KMT2A (MLL) rearrangements: High-risk; particularly common in infants; poor prognosis with standard therapy.
T-Cell ALL (T-ALL)
T-ALL accounts for approximately 15% of ALL cases. It is more common in adolescents and adults than in young children. Key features:
- Frequently presents with a mediastinal (thymic) mass causing respiratory compromise
- Higher white blood cell counts at diagnosis (hyperleukocytosis)
- Historically considered higher risk than B-ALL; now treated with more intensive protocols
- NOTCH1/FBXW7 mutations in ~50–60% — may indicate better prognosis in T-ALL
- NELARABINE: a T-cell-specific nucleoside analog with activity in relapsed/refractory T-ALL
Clinical Presentation of ALL
ALL typically presents acutely, with symptoms developing over days to weeks as bone marrow function deteriorates. Key presenting features include:
- Profound fatigue and pallor from anemia
- Frequent infections from neutropenia — see infections and immune health in leukemia
- Easy bruising and petechiae from thrombocytopenia
- Bone and joint pain — particularly prominent in children, causing limping or refusal to walk (bone pain in leukemia)
- Lymphadenopathy — cervical, axillary, inguinal, and sometimes mediastinal
- Splenomegaly and hepatomegaly causing abdominal fullness
- Night sweats and fever
- CNS symptoms in ~5% at diagnosis: headache, cranial nerve palsies, papilledema (optic disc swelling from raised intracranial pressure)
- In T-cell ALL: mediastinal mass causing breathing difficulty, face/arm swelling (SVC syndrome)
Diagnosing ALL
The diagnostic workup for ALL follows a systematic path:
- CBC with differential: May show markedly elevated WBC (particularly in T-ALL), anemia, thrombocytopenia, and lymphoblasts on peripheral smear. See blood tests in leukemia diagnosis.
- Peripheral blood smear: Lymphoblasts are identified — typically large cells with high nuclear:cytoplasmic ratio, prominent nucleoli, and scant cytoplasm.
- Bone marrow aspirate and biopsy: Required for definitive diagnosis. ALL is defined as ≥20% (or ≥25% by some systems) lymphoblasts in the bone marrow. Learn about bone marrow biopsy.
- Immunophenotyping (flow cytometry): Identifies whether blasts are B-cell (CD19+, CD22+, CD10+) or T-cell (CD3+, CD5+, CD7+) lineage, and the developmental stage.
- Cytogenetics and FISH: Identifies chromosomal abnormalities (hyperdiploidy, Philadelphia chromosome, ETV6-RUNX1, MLL rearrangements).
- Molecular panel (PCR/NGS): Detects specific gene fusions and mutations for risk stratification and to identify targetable alterations.
- Lumbar puncture (LP): CNS evaluation — cerebrospinal fluid analysis for blast cells indicating CNS involvement.
- Imaging: Chest X-ray/CT to assess for mediastinal mass; CT of neck/chest/abdomen/pelvis for disease extent.
For comprehensive guidance on interpreting results, see understanding your leukemia test results.
Treatment of ALL
ALL treatment is delivered in three phases over a period of 2–3 years:
Induction (Weeks 1–4)
The goal of induction is to achieve complete remission (CR) — fewer than 5% blasts in the bone marrow and restoration of normal blood counts. Standard induction regimens combine:
- A corticosteroid (dexamethasone or prednisone)
- A vinca alkaloid (vincristine)
- An anthracycline (doxorubicin, daunorubicin)
- L-asparaginase (pegylated asparaginase)
- For Ph+ ALL: a TKI (dasatinib or ponatinib) is added throughout all phases
CR is achieved in approximately 95% of children and 80–90% of adults after induction.
Consolidation (Months 2–12)
After remission is achieved, consolidation therapy reduces minimal residual disease (MRD) to prevent relapse. This phase typically involves high-dose methotrexate, 6-mercaptopurine, cytarabine, and continuation of the TKI in Ph+ ALL. CNS-directed therapy (intrathecal chemotherapy) is given throughout to prevent CNS relapse, replacing the use of cranial irradiation in most modern protocols.
Maintenance (Months 12–36)
Daily oral 6-mercaptopurine and weekly methotrexate, along with periodic vincristine and steroid pulses, maintain remission during a prolonged 2-year period. For Ph+ ALL, daily TKI continues throughout maintenance.
Stem Cell Transplantation
Allogeneic stem cell transplantation is recommended in first remission for high-risk adult ALL patients (especially Ph+ with inadequate molecular response, T-ALL with unfavorable features) and for all patients in second or subsequent remission after relapse.
Immunotherapy for Relapsed/Refractory ALL
The immunotherapy revolution has dramatically changed outcomes for relapsed ALL:
- Blinatumomab: A bispecific T-cell engager (BiTE) antibody that simultaneously binds CD19 on ALL blasts and CD3 on T cells, directing T cells to kill leukemia cells. FDA-approved for both relapsed/refractory and MRD-positive ALL.
- Inotuzumab ozogamicin: An antibody-drug conjugate targeting CD22, delivering a cytotoxic drug directly to ALL cells. High response rates in relapsed/refractory B-ALL.
- CAR-T cell therapy (tisagenlecleucel — Kymriah): FDA-approved for children and young adults (up to 25 years) with relapsed/refractory B-ALL. Cure rates of approximately 40–60% in heavily pretreated patients. Learn more about immunotherapy.
Prognosis in ALL
ALL prognosis varies significantly by age, subtype, and risk stratification:
| Group | 5-Year Survival | Key Favorable Factors |
|---|---|---|
| Standard-risk children (B-ALL) | >95% | Hyperdiploidy; ETV6-RUNX1; age 1–9; low WBC |
| High-risk children | 70–85% | MLL rearrangement; Ph-like; iAMP21 |
| Adults (ALL) | 35–55% | Age <40; no adverse cytogenetics; MRD negativity |
| Ph+ ALL (adult, with TKI) | 50–60%+ | Deep molecular response; SCT in CR1; ponatinib |
| Relapsed/refractory ALL | 10–40% | Duration of first remission; availability of CAR-T; SCT |
MRD (Minimal Residual Disease) negativity — the absence of detectable leukemia by sensitive PCR or flow cytometry after treatment — is one of the strongest predictors of long-term remission in ALL. Patients who achieve MRD negativity have substantially lower relapse rates. Learn more about MRD testing.
Childhood ALL vs. Adult ALL: Key Differences
The biological and clinical differences between childhood and adult ALL are substantial and drive different treatment approaches. Children tolerate higher-intensity chemotherapy, have more favorable cytogenetic profiles on average, and have organ reserve that allows multi-year intensive treatment. Adults are more likely to have adverse molecular markers (higher rate of Ph+ ALL), reduced organ reserve, and comorbidities that limit treatment intensity. Pediatric-inspired treatment regimens — applying the intensive multi-agent approach used in children — have improved outcomes in young adults (up to age 40). See our full comparison in leukemia symptoms in kids vs. adults and pediatric leukemia care.
Living with ALL During and After Treatment
ALL treatment spans 2–3 years, encompassing major life transitions for both children and adults. Children require educational support, neuropsychological monitoring (particularly with CNS-directed therapy), emotional support, and peer connection programs. Adults may face career disruption, fertility concerns (discuss sperm banking or egg freezing BEFORE starting chemotherapy), and significant financial impact. All patients benefit from multidisciplinary supportive care including oncology social work, psychological support, nutrition consultation, and rehabilitation services. Long-term survivorship care — monitoring for relapse and late effects — is essential after treatment completion.
Caregiver Guidance
ALL treatment is intensive and demands significant caregiver involvement. Transportation to frequent clinic visits, management of medications at home (particularly during maintenance), infection monitoring (immediately seeking care for any fever), nutritional support, and emotional presence are all central caregiver responsibilities. Understanding treatment phases, knowing the specific side effects to watch for at each phase, and maintaining clear communication with the oncology team are essential skills.
When to Seek Emergency Care During ALL Treatment
- Fever above 101°F (38.3°C) — febrile neutropenia is an emergency requiring immediate hospital evaluation
- Any uncontrolled bleeding
- Sudden severe headache or neurological symptoms — possible CNS involvement or intracranial bleed
- Severe shortness of breath — possible mediastinal mass progression or pulmonary infection
- Severe abdominal pain in a child — possible typhlitis
🚨 ALL Treatment Emergencies — Go to the Emergency Room For:
- Fever above 101°F in any phase of treatment
- Severe, sudden headache, confusion, or neurological weakness
- Difficulty breathing or rapidly worsening breathlessness
- Uncontrolled bleeding from any site
💬 Questions to Ask Your ALL Treatment Team
- What is the specific risk category of my ALL and what does it mean for my treatment plan?
- Do I (or my child) have the Philadelphia chromosome, and should a TKI be added?
- What is the MRD result after induction, and what does it predict?
- Should stem cell transplantation be planned in first remission?
- Are there clinical trials available for my specific ALL subtype?
- What late effects should we monitor for after treatment completion?
This content is for informational and educational purposes only. It is not a substitute for professional medical advice, diagnosis, or treatment. Always consult your physician or a qualified healthcare provider with any questions about a medical condition. Never disregard professional medical advice or delay seeking it because of information you have read on this website. Read our full disclaimer.
Frequently Asked Questions
Yes, especially in children. Pediatric ALL has cure rates exceeding 90% with modern intensive chemotherapy protocols.
ALL is the most common childhood cancer, accounting for about 75% of pediatric leukemia diagnoses.
Adult ALL has lower but improving survival rates; modern targeted therapies like blinatumomab and inotuzumab have significantly improved outcomes.
