📋 Quick Summary
- Topic: How leukemia causes weight loss, what counts as unexplained, and when to seek evaluation.
- Key Takeaway: Early recognition and medical consultation are critical for the best clinical outcomes.
- Remember: Always consult a qualified healthcare professional if you have concerns.
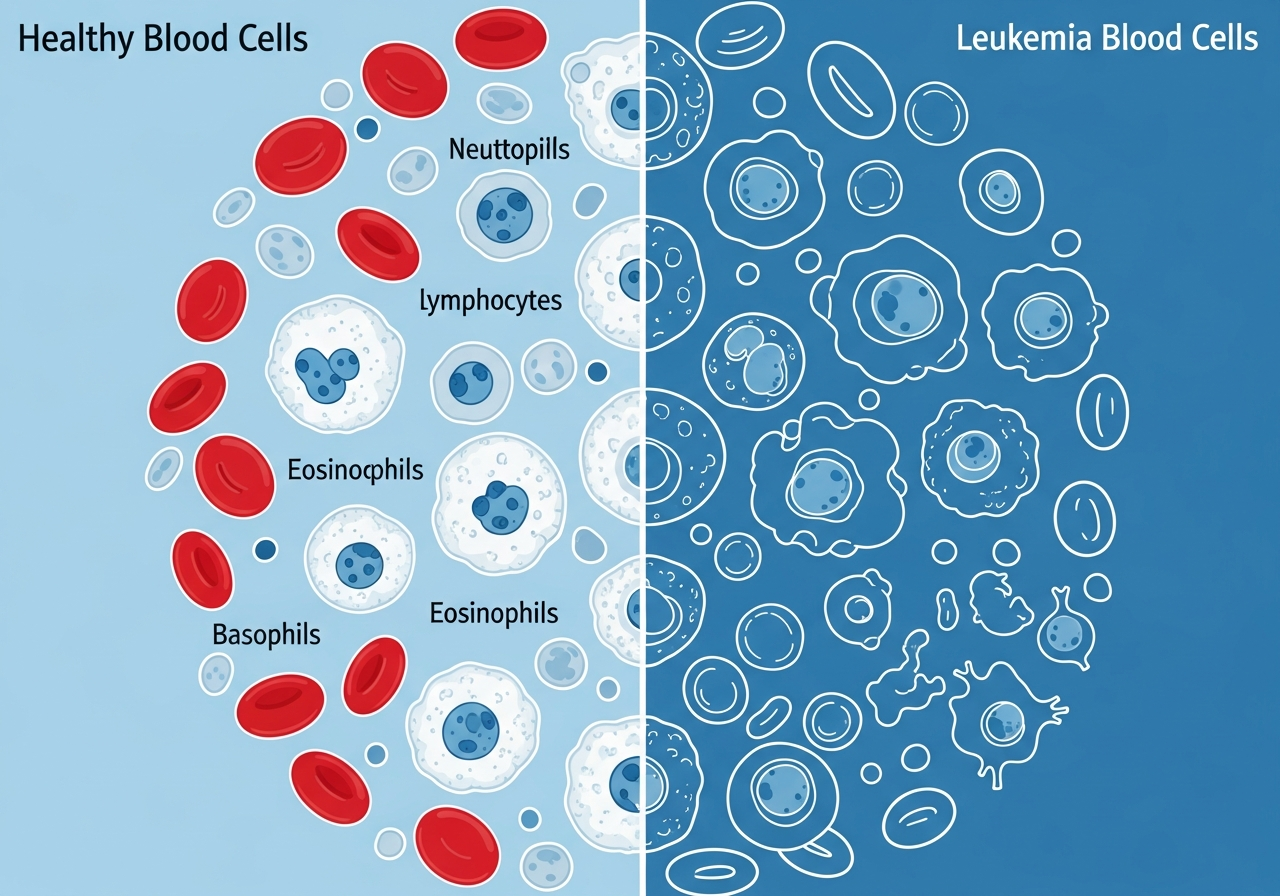
Unexplained Weight Loss and Leukemia
Unexplained weight loss — losing body weight without intentional changes to diet or activity — is one of the classical warning signs of systemic illness, including several types of leukemia and other blood cancers. Clinically, weight loss that is "unexplained" means it cannot be attributed to changes in eating behavior, increased physical activity, or another clearly identified medical cause such as a new thyroid condition or gastrointestinal problem.
In the context of leukemia warning signs, unexplained weight loss carries particular significance when it occurs alongside drenching night sweats and fever — together forming the "B symptom" triad that is associated with more advanced or aggressive hematologic malignancy. Even in isolation, significant unexplained weight loss demands a medical evaluation.
Understanding why leukemia causes weight loss, how much is medically concerning, and how nutritional support is integrated into leukemia treatment helps patients and families respond appropriately to this important but often underappreciated warning sign.
How Leukemia Causes Unexplained Weight Loss
Weight loss in leukemia results from several concurrent processes that accelerate calorie expenditure while simultaneously reducing caloric intake:
Metabolic Drain from Leukemia Cells
Rapidly proliferating leukemia cells have high metabolic demands. They consume glucose, glutamine, and other energy substrates at a rate that exceeds normal tissue requirements. This creates a state of "metabolic competition" — healthy tissues are effectively starved of resources as the leukemia cells commandeer available nutrients. The body responds by breaking down fat stores and, in prolonged cases, lean muscle mass to meet energy demands.
Inflammatory Cytokines and Anorexia
The same cytokines that cause night sweats and fever — including tumor necrosis factor-alpha (TNF-α, historically called "cachectin"), interleukin-1, and interleukin-6 — directly suppress appetite through their effects on the hypothalamus. TNF-α was named "cachectin" because of its role in inducing cachexia (pathological wasting). Even when food is available and a patient is not nauseated, these cytokines create a profound reduction in hunger that results in caloric deficits and weight loss.
Splenomegaly and Early Satiety
In many leukemia types — particularly CML and CLL — leukemia cells accumulate in the spleen, causing it to enlarge dramatically (splenomegaly). The enlarged spleen physically encroaches on the stomach, reducing its functional capacity. Patients feel full after eating very small amounts — a phenomenon called "early satiety" — and involuntarily reduce their food intake. When combined with the cytokine-mediated suppression of appetite, the result is a significant and progressive reduction in caloric intake.
Treatment-Related Factors
During active treatment with chemotherapy, additional causes of weight loss emerge: nausea and vomiting, mouth sores (mucositis), taste changes (dysgeusia), and gastrointestinal inflammation all reduce the ability to eat. While these are treatment-related rather than disease-related, they can compound pre-existing weight loss substantially.
What Counts as Medically Significant Weight Loss
The clinical threshold for "significant" unexplained weight loss is generally accepted as:
- Loss of 5% or more of baseline body weight over 6 to 12 months without intentional dietary restriction or increased activity
- Loss of 10% or more of body weight is considered more severe and is incorporated into the B-symptom definition relevant to staging some lymphocytic leukemias and lymphomas
In practical terms: a 180-pound person losing 9 pounds (5%) over 6 months without trying has crossed the clinical significance threshold. At 18 pounds (10%), the loss is severe and urgently warrants evaluation.
The rate of weight loss is also important. Gradual loss over many months may indicate a chronic, slower-growing malignancy (such as CLL or CML), while rapid weight loss over weeks may indicate a more aggressive acute leukemia or advanced stage of disease. In children, any unexplained weight loss is significant given normal growth expectations — failure to gain weight as expected should raise concern even without absolute weight decline.
Cancer Cachexia: Beyond Simple Weight Loss
In advanced leukemia, unexplained weight loss can progress to a condition called cancer cachexia — a complex metabolic syndrome characterized by ongoing skeletal muscle loss (sarcopenia) with or without loss of fat mass, that cannot be fully reversed by conventional nutritional support alone.
Cachexia is distinct from starvation: in starvation, fat is broken down preferentially to preserve muscle. In cachexia, skeletal muscle is actively catabolized — broken down and consumed — even when caloric intake is maintained. This leads to the profound wasting and weakness that characterizes advanced cancer. The mechanisms involve cytokine-driven protein catabolism, impaired anabolic signaling, and systemic inflammation.
Cancer cachexia is associated with reduced tolerance to treatment, worse treatment outcomes, reduced quality of life, and shorter survival. It is addressed through a combination of nutritional support, anti-inflammatory pharmacological agents, and treatment of the underlying leukemia.
Diagnostic Evaluation of Unexplained Weight Loss
When a patient presents with unexplained weight loss, a systematic evaluation is warranted. In the context of possible leukemia, the key tests include:
- Complete Blood Count (CBC) with differential: The foundational test. Elevated or depressed white cell counts, anemia, or thrombocytopenia point toward bone marrow pathology. See our guide on blood tests in leukemia diagnosis.
- Comprehensive metabolic panel: Evaluates liver and kidney function; elevated LDH (lactate dehydrogenase) is a non-specific marker of rapid cell turnover seen in leukemia.
- Thyroid function (TSH): Hyperthyroidism is a common cause of weight loss that must be excluded.
- Blood glucose: Uncontrolled diabetes can cause significant weight loss through osmotic diuresis.
- Imaging (CT scan): If lymph node or organ enlargement is suspected, CT of the neck, chest, abdomen, and pelvis may reveal organomegaly, lymphadenopathy, or other findings consistent with leukemia or lymphoma.
If the CBC is abnormal or leukemia is strongly suspected clinically, referral to a hematologist and bone marrow biopsy are indicated for definitive diagnosis. Results should be interpreted as described in our guide to understanding leukemia test results.
Treatment and Nutritional Support
The primary approach to weight loss in leukemia is treating the underlying disease. Effective treatment — whether with chemotherapy, targeted therapy, or other modalities — reduces the tumor burden, diminishes cytokine production, and allows appetite to recover. When splenomegaly is contributing to early satiety, spleen reduction through treatment or, in some cases, splenectomy may restore normal meal capacity.
Nutritional support is an essential adjunct to treatment:
- Dietary counseling: A registered dietitian experienced in oncology provides calorie-dense, nutrient-rich eating plans tailored to treatment side effects and individual preferences.
- Oral nutritional supplements: High-calorie, high-protein supplemental drinks (e.g., Ensure, Boost) can supplement dietary intake when full meals are not possible.
- Anti-nausea medications: Effective control of treatment-related nausea with antiemetics allows patients to eat more consistently.
- Appetite stimulants: In some cases, medications such as megestrol acetate or corticosteroids may be used to stimulate appetite, though their use is balanced against other considerations in leukemia patients.
- Enteral or parenteral nutrition: For patients who cannot maintain adequate oral intake, tube feeding (enteral) or intravenous nutrition (parenteral) may be required temporarily during intensive treatment such as stem cell transplantation.
Weight Loss and Prognosis
Significant weight loss at diagnosis is associated with worse outcomes in most cancers, including leukemia. It often correlates with higher disease burden, more aggressive biology, and reduced physiological reserve to tolerate intensive treatment. However, prognosis is determined primarily by the leukemia type, molecular features, and patient age — not by weight loss alone. Many patients with significant weight loss at diagnosis respond well to treatment, regain weight during recovery, and achieve excellent long-term outcomes.
Nutritional Self-Care for Leukemia Patients
Maintaining adequate nutrition during leukemia treatment is one of the most important things patients can do to support their recovery. Practical recommendations include:
- Eat small, frequent meals (5–6 per day) rather than 3 large meals — this is particularly helpful if splenomegaly is causing early satiety
- Prioritize protein-rich foods (eggs, poultry, fish, legumes, dairy) at every meal to preserve muscle mass
- Choose calorie-dense foods during periods of reduced appetite — nuts, avocados, whole-milk dairy, and nut butters add calories in small volumes
- Address taste changes with flavor enhancements — lemon juice, herbs, and varied textures may make food more palatable when chemotherapy alters taste
- Stay well-hydrated — dehydration can suppress appetite and worsen fatigue
- Weigh yourself weekly at the same time of day to track trends and report significant changes to your medical team
Caregiver Guidance
Food preparation and mealtime support are among the most practical and meaningful contributions caregivers can make. Preparing calorie-dense, protein-rich foods in small portions, offering snacks throughout the day rather than relying on formal mealtimes, and gently encouraging eating without pressure all help maintain nutrition. Caregivers should track weight weekly and communicate any significant loss — more than 1–2 pounds per week — to the medical team. Noting whether reduced intake is related to nausea, early satiety, taste changes, or mood may help clinicians identify and address the contributing factor.
When to Seek Medical Attention
Unexplained weight loss warrants prompt medical evaluation (within days to weeks, not months) if:
- 5% or more of body weight has been lost without intentional cause in 6 months or less
- Weight loss is accompanied by fatigue, night sweats, fever, or lymph node swelling
- Weight loss is rapid — more than 1–2 pounds per week on an ongoing basis
In an established leukemia patient, sudden acceleration of weight loss beyond what is expected — particularly with worsening of other symptoms — may indicate disease progression or treatment failure and warrants urgent contact with the oncology team.
🚨 When to Call Your Doctor
- Lost 5%+ of body weight in the past 6 months without explanation
- Rapid weight loss (more than 1–2 lbs/week) on an ongoing basis
- Weight loss with fever, night sweats, or lymph node swelling
- Unable to maintain any oral food or fluid intake for more than 24 hours
💬 Questions to Ask Your Healthcare Team
- How much of my weight loss is attributable to the leukemia versus treatment side effects?
- Should I be referred to a registered dietitian for nutritional counseling?
- What calorie and protein intake should I be targeting each day?
- Are there appetite-stimulating medications that would be appropriate for me?
- At what point would you consider tube feeding or intravenous nutritional support?
- Will my weight stabilize and recover once treatment begins working?
This content is for informational and educational purposes only. It is not a substitute for professional medical advice, diagnosis, or treatment. Always consult your physician or a qualified healthcare provider with any questions about a medical condition. Never disregard professional medical advice or delay seeking it because of information you have read on this website. Read our full disclaimer.
Frequently Asked Questions
Losing 5% or more of body weight over 6–12 months without dietary or lifestyle changes is considered clinically significant.
No — it can result from hyperthyroidism, diabetes, depression, malabsorption, or chronic infection.
Leukemia cells consume large amounts of metabolic energy, and an enlarged spleen presses on the stomach causing early satiety.
