📋 Quick Summary
- Topic: The dominance of ALL in children, specialized treatment centers, managing side effects, and long-term survivorship.
- Key Takeaway: Early recognition and medical consultation are critical for the best clinical outcomes.
- Remember: Always consult a qualified healthcare professional if you have concerns.
Pediatric Leukemia Care: A Comprehensive Family Guide
Leukemia is the most common childhood cancer, and for many families, the diagnosis arrives with devastating suddenness — a child who seemed healthy weeks before is now facing months or years of intensive medical treatment. Despite the shock of diagnosis, the news carries an important counter-narrative: childhood leukemia, particularly Acute Lymphoblastic Leukemia (ALL), is now among the most treatable cancers in modern medicine, with cure rates exceeding 90% in standard-risk patients at specialized pediatric cancer centers. The broader landscape of leukemia types in children is more diverse than in adults — see our overview of leukemia risk across life stages for how childhood and adult presentations differ.
Understanding how pediatric leukemia is treated — the treatment phases, the medications used, the supportive care required, and the long-term concerns for survivors — empowers families to be informed partners in their child's care. It also helps parents recognize which symptoms during treatment require emergency response and which are expected and manageable. The initial signs of leukemia in children are discussed in detail in our comparison of leukemia symptoms in children vs. adults, and the overall symptom picture is covered in our leukemia symptoms resource center.
Pediatric leukemia care differs meaningfully from adult leukemia care in its treatment intensity, the specific chemotherapy agents used, the multi-year duration of therapy, and the attention given to minimizing long-term developmental and neurocognitive effects. Diagnosis is confirmed through blood count testing and a bone marrow biopsy — the same diagnostic pathway used for adults, but with pediatric-specific risk stratification applied to the results. All children with leukemia should be treated at or in consultation with a pediatric cancer center affiliated with cooperative clinical trial groups (such as the Children's Oncology Group, COG).
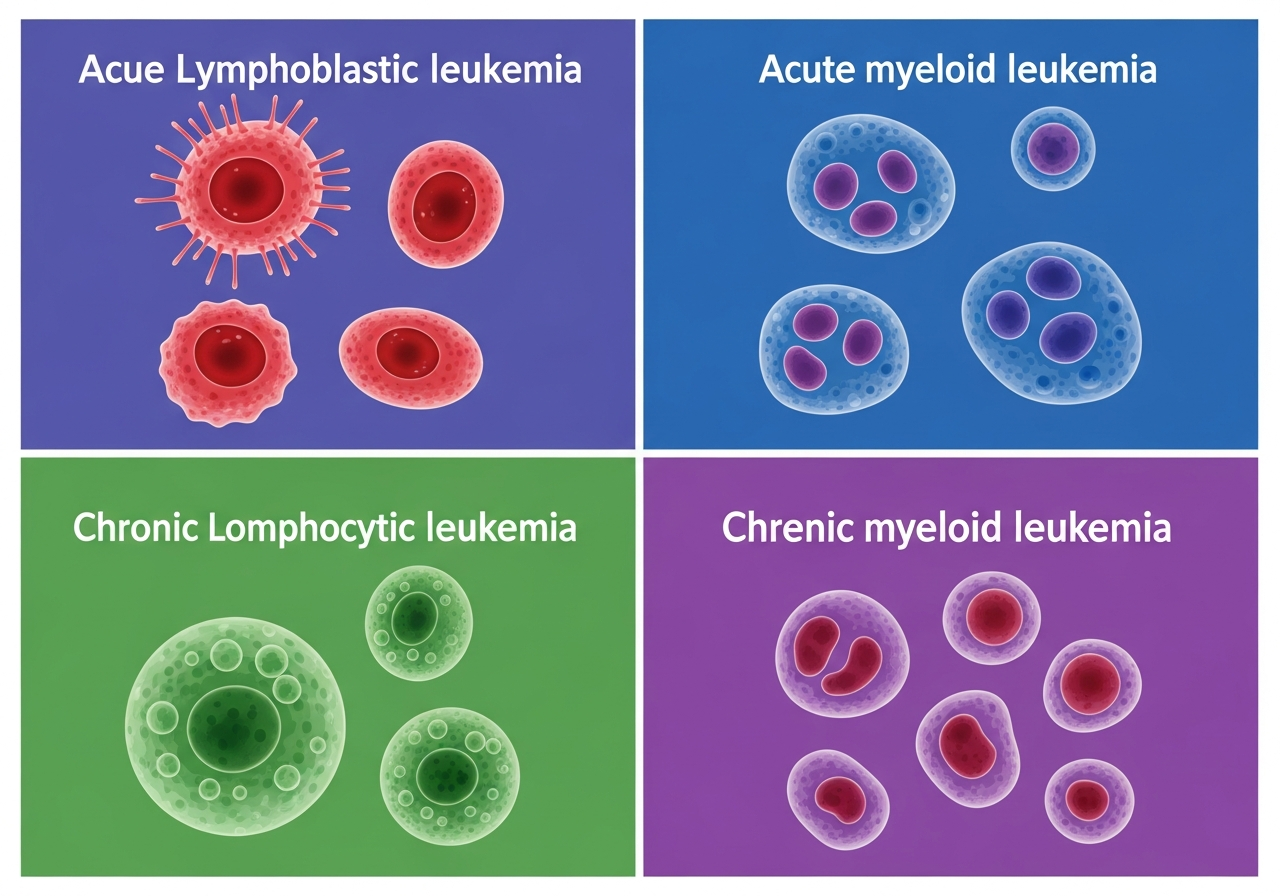
Childhood ALL: The Dominant Diagnosis
Approximately 75–80% of childhood leukemia is ALL (Acute Lymphoblastic Leukemia), with most cases arising from B-lymphocyte precursors (B-ALL). T-cell ALL accounts for approximately 15% and tends to affect older children and adolescents, often with a mediastinal mass and higher white blood cell counts.
Childhood ALL presents most commonly between ages 2 and 5 — a peak that reflects the normal period of intense lymphocyte development during early childhood. Symptoms include profound fatigue and pallor from anemia, bone pain and limping from marrow infiltration, lymph node swelling, bruising and petechiae from thrombocytopenia, and recurrent fever. These symptoms may develop over 2–4 weeks before diagnosis.
Risk stratification in childhood ALL determines treatment intensity:
- Standard risk: Age 1–9.99, initial WBC <50,000/μL, no CNS involvement, rapid initial response — 5-year survival >95%
- High risk: Age ≥10 or WBC ≥50,000/μL; slower initial response; certain cytogenetic features — requires intensified therapy
- Very high risk: Infant ALL (<1 year, particularly with MLL rearrangement); Ph+ ALL; minimal residual disease (MRD) positive after early therapy — most intensive regimens; transplant consideration
Treatment Phases in Childhood ALL
Treatment for childhood ALL is delivered in three sequential phases over approximately 2.5–3 years total:
Phase 1: Induction (Weeks 1–4)
Induction therapy aims to eliminate the vast majority of leukemia cells rapidly and achieve complete remission (less than 5% blasts in the bone marrow). Standard four-drug induction combines:
- Corticosteroid: Dexamethasone or prednisone — powerful anti-leukemia agents; also reduce CNS involvement
- Vincristine: A vinca alkaloid that prevents cell division by disrupting the mitotic spindle
- L-asparaginase (PEG-asparaginase): An enzyme that depletes asparagine — an amino acid leukemia cells cannot synthesize but normal cells can; highly leukemia-selective. Unique side effects include allergy/hypersensitivity, pancreatitis, and thrombosis
- Anthracycline: Doxorubicin or daunorubicin — given in higher-risk patients
Complete remission is achieved in approximately 98–99% of children with standard-risk ALL after induction.
Phase 2: Consolidation (Months 2–8)
Consolidation — also called intensification — delivers additional chemotherapy to eliminate residual leukemia cells (minimal residual disease, MRD) that survive induction. This phase varies by risk group but typically includes:
- High-dose methotrexate with leucovorin rescue — targeting residual disease including CNS compartment
- 6-mercaptopurine (6-MP)
- Additional asparaginase
- Vincristine and steroid pulses
- Intrathecal chemotherapy (see CNS treatment below)
For very high-risk patients (infant ALL, Ph+ ALL), allogeneic stem cell transplantation is considered during consolidation after achieving second remission or for high-risk Ph+ ALL.
Phase 3: Maintenance (Months 8–36)
Maintenance therapy is the longest phase — typically lasting 2–3 years from the start of treatment (or 2 years from the start of maintenance, adjusted by gender). It maintains remission using lower-intensity, predominantly oral chemotherapy:
- 6-mercaptopurine (6-MP): Daily oral dosing — the cornerstone of maintenance. Dose-adjusted based on blood count monitoring
- Methotrexate: Weekly oral dosing
- Vincristine and dexamethasone pulses: Typically every 4 weeks
- Intrathecal chemotherapy: Periodic CNS-directed therapy throughout maintenance
Boys receive longer maintenance than girls (3 years vs. 2 years from start of maintenance) because testicular recurrence is more common without extended treatment.
CNS-Directed Treatment
The CNS is a sanctuary site for leukemia cells — a compartment where systemic chemotherapy penetrates poorly. Without specific CNS-directed therapy, CNS relapse would occur in the majority of patients. Modern protocols use intrathecal chemotherapy (methotrexate and/or cytarabine, delivered directly into the cerebrospinal fluid via lumbar puncture) throughout all treatment phases, administered every few weeks.
Cranial radiation — historically used for CNS prophylaxis — is now reserved only for patients with documented CNS involvement at diagnosis (CNS-3 status, defined as ≥5 blast cells/μL on cytospin) and for very high-risk cases. Eliminating routine cranial radiation from most protocols has dramatically reduced the neurocognitive late effects that plagued survivors treated in the 1970s–1990s, while maintaining equivalent efficacy through intensified systemic and intrathecal chemotherapy.
Supportive Care Throughout Pediatric Leukemia Treatment
Supportive care is the care that keeps patients safe and functional during treatment. For pediatric leukemia, essential supportive care includes:
- Infection prevention and treatment: Prophylactic trimethoprim-sulfamethoxazole (TMP-SMX) for Pneumocystis pneumonia prevention; antifungal prophylaxis; antiviral medications. Febrile neutropenia requires immediate emergency room evaluation. See infections and immune health in leukemia.
- Transfusion support: Red blood cell and platelet transfusions maintain safe hemoglobin and platelet levels during the deepest myelosuppression. All blood products should be irradiated and CMV-safe for pediatric leukemia patients.
- Anti-nausea medications: Antiemetics prevent treatment-related nausea and allow adequate nutrition
- Oral care: Chlorhexidine rinses reduce mucositis-related oral infections
- Nutritional support: Maintaining adequate nutrition during treatment is essential — dietitians experienced in pediatric oncology provide tailored guidance; NG or G-tubes may be required for some patients
- G-CSF (growth factor): May be used in high-risk protocols to shorten neutropenia
- Psychosocial support: Pediatric oncology social workers, child life specialists, and psychologists address the emotional and developmental impact of cancer treatment on children and their families
Prognosis and Survival in Childhood ALL
Childhood ALL represents one of the most remarkable achievements in cancer medicine. Five-year survival rates have risen from less than 10% in the 1960s to over 90% today. Current outcomes by risk group:
- Standard-risk B-ALL: 5-year survival >95%
- High-risk B-ALL: 5-year survival 80–90%
- Very high-risk (infant, Ph+, MRD-positive): 5-year survival 50–75%, improving with newer approaches
- T-cell ALL: 5-year survival 75–85% with intensified protocols
Approximately 80% of children diagnosed with ALL are cured — meaning they achieve long-term remission without relapse. The children who relapse face a much harder road — second remissions are achievable but second cure rates are lower. New immunotherapy agents (blinatumomab, inotuzumab, CAR-T cell therapy) have dramatically improved outcomes for relapsed/refractory childhood ALL.
Long-Term Survivorship: Life After ALL
More than 90% of children treated for ALL are long-term survivors, and the population of childhood cancer survivors in the United States now exceeds 500,000. Survivorship care — the medical monitoring and support provided after active treatment ends — is an essential and rapidly expanding component of pediatric oncology.
Childhood leukemia survivorship encompasses:
- Relapse surveillance: Regular CBC monitoring and, for higher-risk patients, MRD surveillance by PCR — most intensive in the first 2 years after treatment completion
- Late effects monitoring: Systematic assessment for the delayed health consequences of chemotherapy and radiation (see below)
- Developmental monitoring: Neurocognitive assessment, academic progress tracking, and behavioral health evaluation
- Reproductive health: Assessment of fertility implications of chemotherapy received, and counseling for adolescent survivors
- Cardiovascular monitoring: Anthracyclines (doxorubicin, daunorubicin) increase lifetime risk of cardiomyopathy; regular echocardiogram surveillance is standard
Late Effects of Childhood Leukemia Treatment
The long-term effects of childhood leukemia treatment are a significant survivorship concern. Extensive research through the Childhood Cancer Survivor Study (CCSS) has characterized these effects:
- Neurocognitive effects: Even without cranial radiation, intrathecal methotrexate can cause subtle deficits in processing speed, attention, and working memory. These are most significant in children treated at younger ages. Early educational intervention and academic support minimize functional impact.
- Cardiovascular effects: Anthracycline cardiotoxicity (cardiomyopathy) — risk increases with cumulative dose; left ventricular dysfunction may manifest decades after treatment. Annual echocardiogram monitoring is recommended for patients who received significant anthracycline exposure.
- Endocrine effects: Growth hormone deficiency (particularly after cranial radiation); obesity and metabolic syndrome; thyroid dysfunction; adrenal insufficiency (from prolonged steroid use)
- Bone health: Osteopenia and osteonecrosis (avascular necrosis) — particularly from corticosteroids; more common in adolescents and those receiving dexamethasone
- Secondary malignancies: A 5–10x increased risk of second cancers in the decades following treatment — particularly brain tumors (post-cranial radiation), bone sarcomas, and therapy-related AML
- Psychological effects: Post-traumatic stress, health anxiety, and depression are more common in childhood cancer survivors than in the general population; access to mental health services in survivorship clinics is essential
Family and Patient Support During Treatment
Childhood leukemia affects the entire family. Key resources and support mechanisms include:
- Pediatric oncology social workers: Available at all pediatric cancer centers; provide counseling, connect families to financial assistance programs, assist with insurance navigation, and support siblings and parents
- Child life specialists: Child development experts embedded in pediatric oncology who help children understand and cope with procedures, maintain developmentally appropriate activities, and prepare siblings
- School liaison programs: Many pediatric cancer centers have school liaison staff who coordinate with the child's school district to maintain educational connection during treatment
- Parent support groups: Peer connections with other families who have navigated pediatric leukemia provide validation, practical advice, and community
- Organizations: The Leukemia & Lymphoma Society (LLS), Alex's Lemonade Stand Foundation, and similar organizations provide both financial assistance and family education resources
Caregiver and Parent Guidance
Parents caring for a child with leukemia face extraordinary practical and emotional demands. Key priorities:
- Understand the fever rule: Any fever above 101°F (38.3°C) in a child on chemotherapy is a medical emergency requiring immediate hospital evaluation — do not give fever-reducing medication and wait. Call your oncology team and go to the nearest emergency room.
- Maintain vaccination schedules for siblings and household contacts: Household members should receive influenza vaccine annually. Live vaccines (MMR, varicella) in household contacts of severely immunocompromised patients require team guidance.
- Track medications carefully: Maintenance therapy involves daily oral medications (6-MP and weekly methotrexate) that must be given correctly and consistently. Missed doses increase relapse risk; overdoses cause toxicity.
- Attend all follow-up appointments: Blood count monitoring, MRD testing, and regular clinical assessment are not optional — they detect treatment failure early when intervention is most effective.
- Care for caregiver wellbeing: Caregiver burnout is common and can compromise the quality of care. Respite care, peer support, and mental health resources for parents are legitimate and important.
When to Seek Emergency Care During Childhood Leukemia Treatment
- Fever above 101°F (38.3°C) — febrile neutropenia is always an emergency in children receiving leukemia treatment
- Child is unresponsive, confused, or having a seizure
- Significant bleeding that does not stop with sustained pressure
- Severe abdominal pain — possible typhlitis (neutropenic enterocolitis)
- Difficulty breathing or rapidly worsening respiratory status
- Severe headache, vomiting in the morning, or vision changes — possible CNS involvement
🚨 When to Go to the Emergency Room During Childhood Leukemia Treatment
- Fever above 101°F (38.3°C) — do not wait, go immediately
- Child unresponsive, having a seizure, or experiencing sudden neurological change
- Uncontrolled bleeding from any site
- Severe abdominal pain with fever (possible typhlitis)
- Breathing difficulty or rapid respiratory deterioration
💬 Questions to Ask Your Child's Leukemia Treatment Team
- What risk group is my child in, and what does that mean for treatment intensity and duration?
- What is the MRD result after induction, and what does it predict about my child's prognosis?
- Are there clinical trials available that my child should be enrolled in?
- What late effects should we monitor for after treatment ends, and when?
- How do I handle a fever at home — what temperature triggers an ER visit?
- What educational support services are available for my child during and after treatment?
This content is for informational and educational purposes only. It is not a substitute for professional medical advice, diagnosis, or treatment. Always consult your physician or a qualified healthcare provider with any questions about a medical condition. Never disregard professional medical advice or delay seeking it because of information you have read on this website. Read our full disclaimer.
Frequently Asked Questions
Overall 5-year survival for pediatric leukemia exceeds 85–90%, with ALL having the highest rates at over 90%.
Treatment involves chemotherapy delivered over 2–3 years in phases; radiation and transplant are used selectively.
Survivors may face learning difficulties, cardiac issues, growth problems, and increased risk of secondary cancers, requiring lifelong monitoring.
