📋 Quick Summary
- Topic: Lymph node anatomy, why leukemia causes swelling, and how to distinguish cancer-related swelling from infection.
- Key Takeaway: Early recognition and medical consultation are critical for the best clinical outcomes.
- Remember: Always consult a qualified healthcare professional if you have concerns.
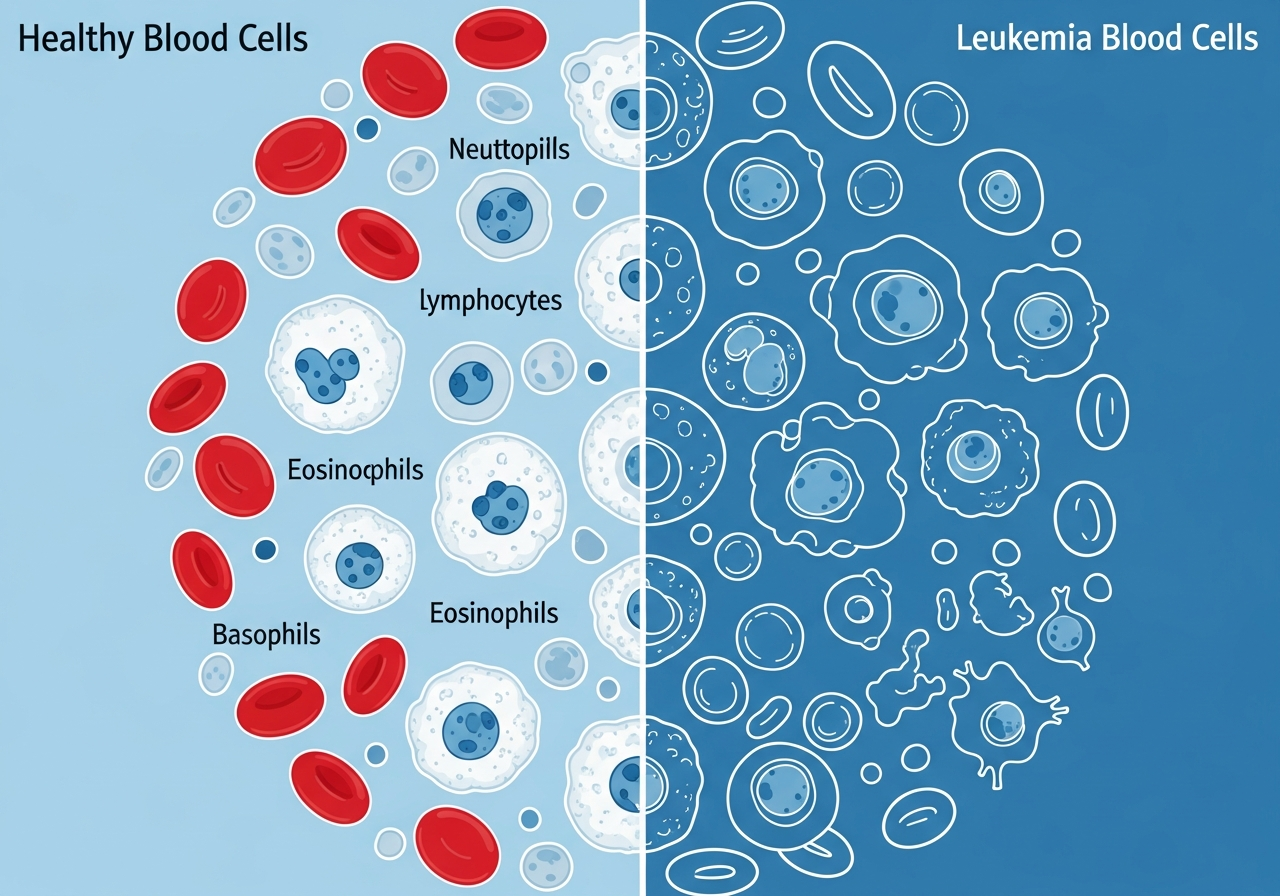
Swollen Lymph Nodes and Leukemia
Lymph node enlargement (lymphadenopathy) is one of the most recognizable and frequently reported findings in several types of leukemia. While swollen lymph nodes are an extremely common and usually benign response to infection, persistent, painless, firm lymph node enlargement — particularly when accompanied by other leukemia warning signs — requires medical evaluation.
In lymphocytic leukemias — particularly Chronic Lymphocytic Leukemia (CLL) and Acute Lymphoblastic Leukemia (ALL) — the leukemia cells are derived from lymphocytes, the very cell type that normally resides in and transits through lymph nodes. When these cells undergo malignant transformation, they accumulate in lymph nodes, causing progressive enlargement that can become clinically significant.
Understanding the difference between infection-related and malignancy-related lymph node swelling, where to look, and what features should prompt medical evaluation is essential knowledge for patients and their families.
The Lymphatic System and Lymph Node Function
The lymphatic system is a network of vessels and nodes that runs throughout the body, playing a central role in immune function and fluid balance. Lymph nodes — small, bean-shaped organs ranging from a few millimeters to about 1 centimeter in diameter — serve as filters and immune activation centers. When pathogens or abnormal cells enter the lymphatic circulation, lymph nodes trap and present them to immune cells (lymphocytes), triggering an immune response.
There are hundreds of lymph nodes throughout the body, clustered in specific regions:
- Cervical (neck): Most commonly palpable during upper respiratory infections; also involved in lymphocytic leukemias
- Axillary (armpits): Common location for lymphadenopathy in CLL
- Inguinal (groin): Enlarged in lower body infections and many leukemia/lymphoma presentations
- Mediastinal (chest): Not directly palpable but visible on imaging; enlarged in T-cell ALL and lymphomas
- Abdominal/retroperitoneal: Also not palpable but clinically important in CLL and lymphomas
Under normal circumstances, lymph nodes respond to infection by temporarily enlarging as immune cells proliferate to mount a defense. They then return to normal size once the infection resolves — typically within 2–6 weeks. Lymph nodes that remain enlarged beyond this timeframe, or that enlarge without an identifiable infection, require investigation.
How Leukemia Causes Lymph Node Swelling
In lymphocytic leukemias, malignant lymphocytes accumulate in lymph nodes through several mechanisms:
- Homing and trafficking: Leukemic lymphocytes, like their normal counterparts, express surface receptors (homing receptors such as CD44 and CD62L) that direct them to lymph nodes. This normal lymphocyte behavior, now occurring with malignant cells, drives their accumulation in nodal tissue.
- Impaired apoptosis: Normal lymphocytes die after completing an immune response (programmed cell death / apoptosis). Leukemic lymphocytes have genetic defects that prevent apoptosis, allowing them to accumulate indefinitely within lymph nodes.
- Microenvironment support: The lymph node microenvironment provides growth signals (from stromal cells, T-helper cells, and accessory cells) that are co-opted by leukemia cells to promote their survival and proliferation.
The degree of lymphadenopathy varies significantly by leukemia type. In CLL, lymph node enlargement may be modest initially but can become massive (bulky lymphadenopathy) in advanced disease. In ALL, lymphadenopathy is typically present at diagnosis and regresses quickly with effective chemotherapy. In AML, significant lymphadenopathy is less common because myeloid leukemia cells do not home to lymph nodes as readily as lymphocytic cells.
Clinical Presentation of Leukemia-Associated Lymphadenopathy
The characteristics that distinguish leukemia-related lymph node swelling from benign (infection-related) swelling are clinically important:
- Painlessness: Leukemia-related nodes are typically painless. Infection-related nodes are usually tender to touch. Painlessness in a swollen node is a "red flag" feature.
- Firmness: Leukemia nodes are often firm or rubbery (described as "rubbery" in CLL and lymphomas). Infection nodes tend to feel softer and fluctuant.
- Persistence: Remains enlarged beyond 2–6 weeks, long after any possible infection has resolved.
- Progressive enlargement: Grows larger over time rather than resolving.
- Multiple sites: Leukemia-related lymphadenopathy often involves multiple node groups (generalized lymphadenopathy), whereas infection usually causes localized nodal swelling in the region draining the infected area.
- No overlying skin changes: Unlike an abscess, leukemia nodes rarely show redness, warmth, or skin breakdown over them.
In CLL, lymph node enlargement may be subtle and asymptomatic for years. In ALL, nodes may be dramatically enlarged at diagnosis — with mediastinal lymphadenopathy causing breathing difficulty from airway compression. Abdominal lymphadenopathy may contribute to abdominal fullness and discomfort.
Distinguishing Cancer-Related from Infection-Related Swelling
| Feature | Infection-Related | Leukemia/Malignancy-Related |
|---|---|---|
| Tenderness | Usually tender / painful | Usually painless |
| Consistency | Soft, fluctuant | Firm, rubbery |
| Duration | Resolves within 2–6 weeks | Persistent; may grow progressively |
| Associated illness | Sore throat, fever, local infection | Fatigue, night sweats, weight loss |
| Number of sites | Typically one region | Often multiple (generalized) |
| Response to antibiotics | Usually resolves | Does not resolve |
A simple but practical clinical rule: a lymph node that does not return to normal size within 2–4 weeks after an infection has resolved warrants medical evaluation, particularly if it is painless, firm, and larger than 1 centimeter in diameter. Any painless node larger than 2 centimeters requires urgent evaluation regardless of timing.
Diagnostic Evaluation of Lymphadenopathy
When enlarged lymph nodes raise concern, the evaluation typically proceeds as follows:
- History and physical examination: The physician will assess node characteristics (size, consistency, tenderness, mobility, location), look for signs of infection, and screen for systemic leukemia symptoms.
- Complete blood count (CBC): The CBC with differential is essential. In CLL, a markedly elevated lymphocyte count (absolute lymphocyte count typically above 5,000–10,000 cells/μL, with small mature-appearing lymphocytes) is often diagnostic. In ALL, blast cells on peripheral smear confirm the diagnosis.
- CT scan: Provides detailed information about the extent of lymphadenopathy — including nodes not clinically palpable in the chest, abdomen, and pelvis.
- PET scan: Useful in lymphomas; less routine in CLL; may be used in ALL staging.
- Lymph node biopsy: In some cases — particularly when distinguishing CLL from lymphoma — a lymph node biopsy provides definitive histopathology and immunophenotyping.
- Bone marrow biopsy: Central to confirming the diagnosis and extent of bone marrow involvement in any leukemia. Learn more about bone marrow biopsy.
How Treatment Affects Lymphadenopathy
In ALL, lymphadenopathy responds rapidly to induction chemotherapy — nodes typically shrink dramatically within weeks of treatment initiation. This rapid nodal response is one of the hallmarks of chemosensitive disease.
In CLL, nodal response depends on the treatment used. BTK inhibitors (ibrutinib, acalabrutinib, zanubrutinib) often cause a transient early increase in lymphocyte count (lymphocytosis) as cells are mobilized from nodes into the blood, followed by gradual reduction in lymph node size over months. BCL-2 inhibitors (venetoclax) typically produce more rapid nodal reduction. The choice between these targeted therapies depends on the patient's molecular profile and comorbidities.
Prognosis and Lymphadenopathy
In CLL, the degree of lymphadenopathy is incorporated into the Rai and Binet staging systems. Bulky lymphadenopathy (nodes larger than 5–10 cm) indicates higher-stage disease and may prompt earlier treatment initiation. In ALL, the degree of lymphadenopathy at diagnosis is one component of risk stratification but is less determinative than cytogenetic and molecular features. The overall prognosis reflects the specific leukemia type and molecular biology more than the degree of lymphadenopathy alone.
Self-Monitoring for Lymph Node Changes
Patients who are aware of enlarged lymph nodes — whether newly diagnosed or in follow-up — benefit from periodic self-examination. The most accessible nodes are in the neck, armpits, and groin. Monthly self-examination at the same time allows patients to notice significant changes in size, texture, or the appearance of new nodes, which should be reported to the medical team. Patients on watchful waiting for CLL are particularly encouraged to perform monthly self-checks and report any node that has doubled in size within two months.
Caregiver Guidance
Caregivers who notice neck, armpit, or groin swelling that the patient has not mentioned, or who observe increasing abdominal girth that may reflect internal node enlargement, should encourage the patient to report these findings at the next medical appointment — or sooner if nodes are rapidly enlarging. A mediastinal node mass causing visible facial or arm swelling, or breathing difficulty that worsens when lying flat, is an emergency that requires immediate medical contact.
When to Seek Medical Evaluation
- Any painless, firm lymph node that persists for more than 2–3 weeks
- A node larger than 2 centimeters in diameter
- Multiple enlarged nodes in different body regions
- Any lymph node swelling accompanied by unexplained fatigue, night sweats, or weight loss
- Rapidly enlarging nodes — doubling in size over 2 months or less
- Facial or arm swelling with a chest mass (suggests SVC syndrome — emergency)
- Breathing difficulty that worsens when lying flat (suggests mediastinal mass — emergency)
🚨 Seek Emergency Care For:
- Swelling of the face, neck, or arms alongside a chest mass (Superior Vena Cava syndrome)
- Shortness of breath that worsens when lying flat (possible mediastinal compression)
- Audible stridor or high-pitched breathing sounds
💬 Questions to Ask Your Healthcare Team
- How large are my lymph nodes and have they changed since my last visit?
- Do I need imaging to assess nodes I cannot feel myself?
- Is a lymph node biopsy needed to confirm or characterize my diagnosis?
- How will my treatment affect the size of my lymph nodes?
- What rate of nodal growth would indicate that my disease is progressing?
- Should I be performing monthly self-examination, and what changes warrant a call to your office?
This content is for informational and educational purposes only. It is not a substitute for professional medical advice, diagnosis, or treatment. Always consult your physician or a qualified healthcare provider with any questions about a medical condition. Never disregard professional medical advice or delay seeking it because of information you have read on this website. Read our full disclaimer.
Frequently Asked Questions
No — lymph nodes frequently swell during minor infections like colds or strep throat as a normal immune response.
They commonly appear in the neck, armpits, or groin. Unlike infection-related nodes, leukemia-related nodes are typically painless and firm.
If a node remains enlarged for more than two weeks, grows larger, feels hard or rubbery, or is painless, consult a physician.
