📋 Quick Summary
- Topic: Why leukemia causes bone and joint pain, what bone marrow involvement means, and how it differs from arthritis.
- Key Takeaway: Early recognition and medical consultation are critical for the best clinical outcomes.
- Remember: Always consult a qualified healthcare professional if you have concerns.
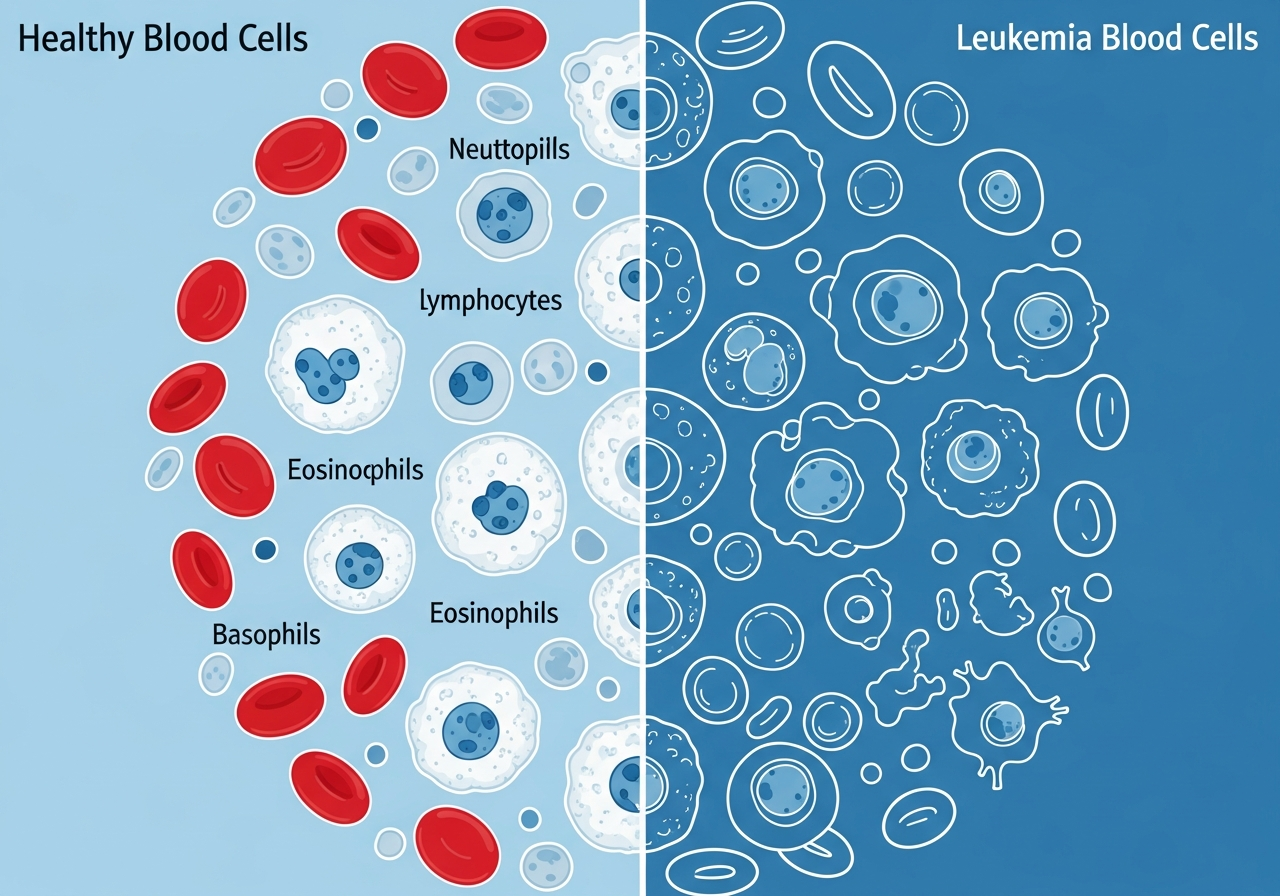
Bone Pain, Bone Health, and Leukemia
Bone pain is an underrecognized but clinically important symptom of leukemia — particularly in Acute Lymphoblastic Leukemia (ALL) and, to a lesser extent, AML. It arises when leukemia cells proliferate within the bone marrow and exert increasing pressure on the bone itself, stimulating pain receptors in the highly innervated periosteum (the bone's outer membrane).
Leukemia-related bone pain is one of the most diagnostically important symptoms in pediatric oncology. In children, it is often severe, multifocal, and the primary symptom that triggers medical evaluation. In adults, bone pain from leukemia is less prominent but still occurs and may be misattributed to arthritis, injury, or musculoskeletal disease — delaying diagnosis.
Recognizing bone pain as a potential leukemia symptom — rather than a musculoskeletal problem — and connecting it to other early leukemia warning signs such as fatigue, pallor, and bruising is key to prompt diagnosis and early treatment.
Why Leukemia Causes Bone and Joint Pain
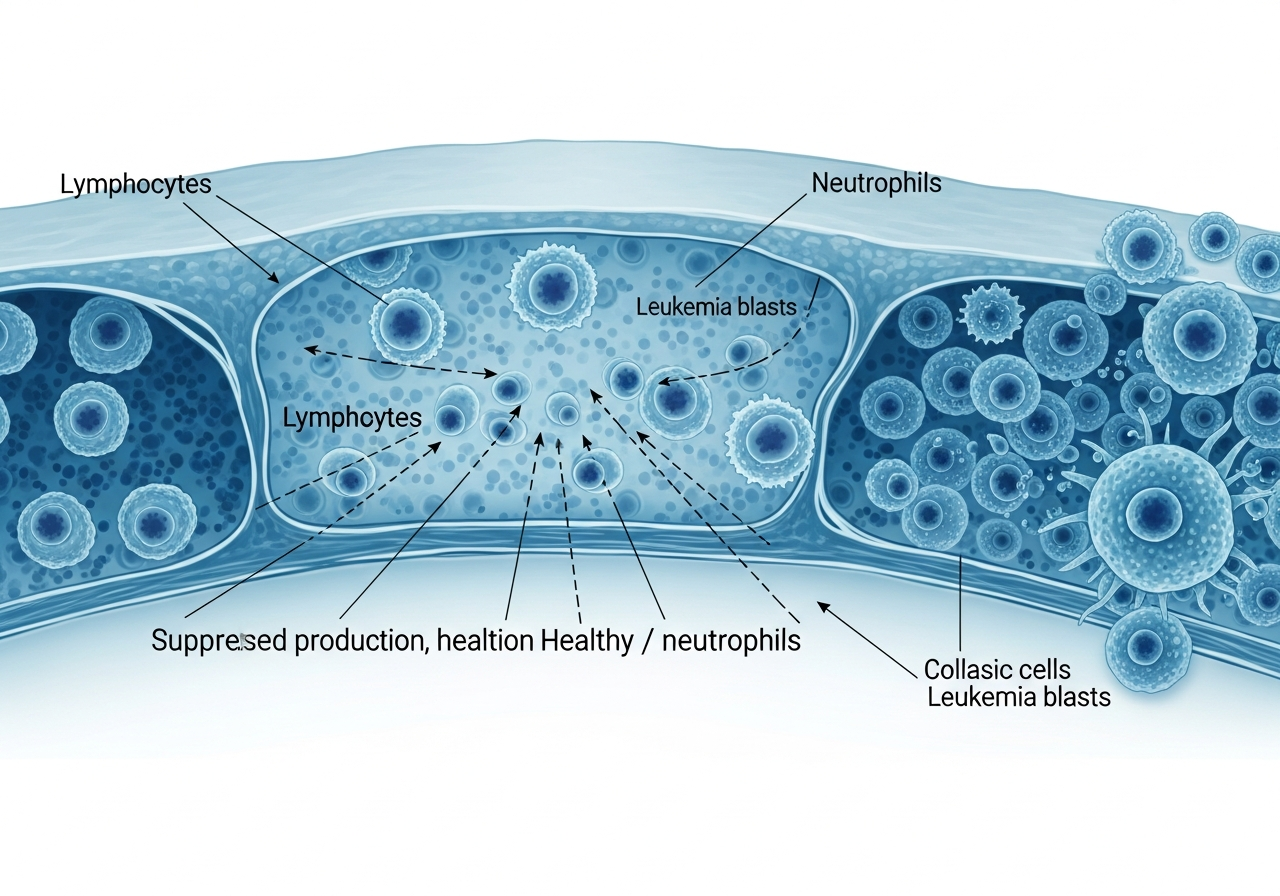
The bone marrow is the primary site of leukemia development. As leukemia cells expand within this confined space, they cause bone pain through multiple mechanisms:
Periosteal Expansion and Stretching
The periosteum — the dense fibrous membrane that covers the outer surface of all bones — is richly supplied with pain receptors (nociceptors). When leukemia cells accumulate in such large numbers that the marrow cavity expands beyond its normal boundaries, the periosteum is stretched. This periosteal distension generates a characteristic deep, aching pain that may worsen at night when the patient is lying still (limiting distraction from the pain) and with direct pressure on the bone.
Cortical Bone Infiltration
In more advanced marrow infiltration, leukemia cells can directly invade the cortical bone (the hard outer shell of the bone), causing lytic (destructive) lesions. This structural weakening can increase pain intensity and, rarely, can predispose to pathological fractures — breaks occurring without significant trauma. Cortical involvement is more common in myeloma than in leukemia, but it can occur in high-burden leukemia.
Joint Involvement and Synovitis
Leukemia cells can infiltrate the synovium (joint lining), producing leukemic arthritis — inflammation and pain within the joint space that closely mimics rheumatological conditions. This is one of the reasons childhood leukemia is so frequently misdiagnosed as juvenile idiopathic arthritis in its early stages. Unlike septic arthritis (joint infection), leukemic arthritis is typically non-destructive and resolves rapidly with leukemia treatment.
Cytokine-Mediated Pain
Beyond direct infiltration, the inflammatory cytokines released by leukemia cells and by the immune system's response to them sensitize pain pathways throughout the body. This central and peripheral sensitization contributes to a diffuse aching and heightened pain sensitivity that makes even normally non-painful activities uncomfortable.
Clinical Presentation of Bone Pain in Leukemia
Leukemia-related bone pain has several clinical characteristics:
- Location: Most commonly in the long bones of the lower extremities (femur, tibia), the spine, the sternum, and the ribs — sites of active red marrow in both children and adults. Pain is often bilateral and affects multiple sites.
- Character: Deep, aching, or throbbing — not sharp or stabbing unless bone destruction has occurred. May be described as a "toothache-like" pain within the bone.
- Timing: Often worse at night and in the early morning — when patients are still and prone to being aware of the pain. May also worsen with activity or direct pressure on the bone.
- Association with other symptoms: Rarely occurs in isolation — typically accompanied by fatigue, pallor, lymph node swelling, or night sweats.
- In children: May present as limping, refusal to walk, refusal to climb stairs, or generalized irritability and reluctance to move. Children often point to their legs or hips when asked where it hurts.
- In adults: May be attributed to arthritis, osteoporosis, or work-related musculoskeletal strain — careful history-taking and physical examination are needed to identify the pattern as systemic rather than mechanical.
Distinguishing Leukemia Bone Pain from Other Causes
| Condition | Distinguishing Features |
|---|---|
| Leukemia (ALL/AML) | Deep, bilateral, multifocal; night pain; fatigue; pallor; abnormal CBC |
| Growing pains (children) | Usually calf/thigh; bilateral; no daytime symptoms; normal blood work; normal physical exam |
| Juvenile idiopathic arthritis | Joint swelling; morning stiffness; positive ANA/RF; normal CBC; no blast cells |
| Osteoarthritis (adults) | Joint-specific; worse with activity; X-ray shows joint space narrowing; normal CBC |
| Osteomyelitis (bone infection) | Localized; fever; elevated ESR/CRP; MRI shows marrow edema and abscess |
| Multiple myeloma | Age >50; spine and ribs; lytic lesions on X-ray; elevated protein; different blood count pattern |
| Metastatic cancer to bone | Known primary cancer history; bone scan positive; abnormal alkaline phosphatase |
The key distinguishing features of leukemia bone pain are: multifocal (affecting multiple bones simultaneously), presence of systemic symptoms (fatigue, fever, night sweats), and — most critically — an abnormal complete blood count. Any child with unexplained bone pain should have a blood count performed before attributing the pain to growing pains or benign musculoskeletal causes.
Diagnostic Evaluation of Bone Pain in Suspected Leukemia
The workup for bone pain potentially related to leukemia includes:
- CBC with differential: The essential first test. In leukemia, this may show anemia (low hemoglobin), thrombocytopenia (low platelets), and elevated or low white blood cell counts. Blast cells visible on peripheral smear are diagnostic. See our guide to blood tests in leukemia diagnosis.
- ESR and CRP: Markers of inflammation — often mildly elevated in leukemia but dramatically elevated in osteomyelitis and autoimmune arthritis.
- Uric acid and LDH: Both may be elevated in leukemia from rapid cell turnover — elevated LDH in particular suggests high proliferative activity.
- X-rays: May show periosteal reaction, lytic lesions, or osteopenia in leukemia, but X-rays are often normal in early disease. Characteristic "leukemia lines" — transverse metaphyseal lucent bands — may be visible in children.
- MRI: The most sensitive imaging for detecting marrow infiltration. MRI of the whole body or affected region shows characteristic replacement of normal marrow signal by leukemia cells. Highly informative in ambiguous cases.
- Bone marrow biopsy: The definitive test that confirms leukemia diagnosis, identifies the specific type, and guides treatment. Read more about what to expect from bone marrow biopsy.
Treatment of Bone Pain in Leukemia
Disease Treatment
The definitive treatment for leukemia-related bone pain is treating the underlying leukemia. As chemotherapy reduces the leukemia cell burden in the bone marrow, periosteal pressure decreases and bone pain typically resolves rapidly — often within days to a few weeks of starting treatment. This rapid pain resolution is often one of the first therapeutic milestones that leukemia patients experience and is a strong indicator that the treatment is working.
Pain Management During the Diagnostic Period
Prior to or during early treatment, pain management is essential. Options include:
- Acetaminophen (paracetamol): First-line analgesic — effective and safe, without the antiplatelet effects of NSAIDs that could worsen bleeding in thrombocytopenic patients.
- NSAIDs (ibuprofen, naproxen): Generally avoided in leukemia patients due to platelet inhibition, increasing bleeding risk in an already thrombocytopenic patient. Use only under medical guidance if clearly indicated.
- Opioid analgesics: For severe bone pain that does not respond to acetaminophen, short-term opioids (oxycodone, hydrocodone, morphine) may be used under close medical supervision.
- Corticosteroids: These are frequently part of leukemia treatment regimens (dexamethasone, prednisone in ALL protocols) and have a rapid anti-inflammatory effect that reduces bone pain as a side benefit of disease treatment.
Bone Health Considerations During Treatment
Corticosteroids, used extensively in ALL treatment, suppress osteoblast activity and increase fracture risk. Calcium and vitamin D supplementation are standard recommendations for patients on prolonged steroid therapy. In some protocols, bisphosphonate therapy (zoledronate) may be considered to preserve bone density during intensive steroid use.
Bone Pain as a Prognostic Indicator
Interestingly, in pediatric ALL, the presence of bone pain at diagnosis has been historically associated with a more favorable prognosis. This is thought to reflect a specific biological subtype of ALL (hyperdiploidy — cells containing extra chromosomes) that both produces prominent bone pain and responds particularly well to chemotherapy. The association is not absolute, however, and bone pain alone cannot be used for prognostic stratification, which requires molecular and cytogenetic analysis.
Living with Bone Pain During Leukemia Diagnosis and Treatment
Bone pain can be one of the most disabling aspects of the early leukemia experience — particularly for children and for adults managing the pain alongside a new, frightening diagnosis. Key strategies for managing bone pain include:
- Discuss all analgesic options with the oncology team — there is no value in suffering pain unnecessarily during a diagnostic period
- Heat pads may provide temporary relief for localized bone pain between analgesic doses
- Limit weight-bearing if bone pain is severe — discuss activity restrictions with your medical team
- Communicate the severity, location, and character of bone pain precisely — "which bone," "scale of 1–10," and "worse at night or during the day" helps the team assess whether the pain is responding to treatment
- Once treatment begins, track whether the pain is improving — early pain reduction is a reassuring sign of treatment response
Caregiver Guidance
For parents of children with leukemia: it is appropriate and important to advocate clearly for adequate pain relief for your child. Children in pain cannot participate fully in the diagnostic process, sleep adequately, or maintain the nutritional intake needed to support treatment. Pain management is a medical priority equal to other aspects of leukemia care. Help your child describe their pain by using a pain scale with faces or numbers, and communicate your observations about nighttime waking, walking difficulties, and behavioral changes to the clinical team.
When to Seek Medical Evaluation for Bone Pain
- Deep, aching, multifocal bone pain in a child — particularly if accompanied by pallor, bruising, or unusual fatigue — requires urgent medical evaluation and a CBC
- Any adult with unexplained bone pain lasting more than 2–3 weeks, particularly with systemic symptoms (fatigue, night sweats, weight loss) warrants evaluation
- Severe bone pain with sudden onset may indicate a pathological fracture — requires emergency imaging
- In a patient already diagnosed with leukemia: new, severe bone pain during treatment — particularly if accompanied by fever — may indicate infection (osteomyelitis) or disease progression
🚨 Urgent Bone Pain Warning Signs
- Child refusing to walk with pallor and unexplained bruising — urgent CBC needed
- Sudden severe bone pain possibly indicating fracture — emergency imaging
- Bone pain with fever in a leukemia patient — possible osteomyelitis or sepsis
💬 Questions to Ask Your Healthcare Team
- Could my (or my child's) bone pain be coming from leukemia cell infiltration of the marrow?
- Should I avoid NSAIDs given the risk of bleeding in leukemia?
- Do I need an MRI to assess the extent of bone involvement?
- How quickly does bone pain typically improve after starting chemotherapy?
- Are there bone density concerns I should be aware of given the treatment plan?
- What pain relief is safe to take at home before my next appointment?
This content is for informational and educational purposes only. It is not a substitute for professional medical advice, diagnosis, or treatment. Always consult your physician or a qualified healthcare provider with any questions about a medical condition. Never disregard professional medical advice or delay seeking it because of information you have read on this website. Read our full disclaimer.
Frequently Asked Questions
No — bone pain is most commonly caused by injuries, arthritis, or growing pains. Deep, aching bone pain without a clear cause warrants investigation.
Pain typically occurs in long bones (legs and arms), ribs, and the sternum, where active bone marrow is concentrated.
Yes — as treatment reduces the cancer cell burden in the marrow, pressure decreases and bone pain generally resolves over time.
