📋 Quick Summary
- Topic: What CMML is, its overlap with MDS and MPN, treatment options, and prognosis for this rare blood cancer.
- Key Takeaway: Early recognition and medical consultation are critical for the best clinical outcomes.
- Remember: Always consult a qualified healthcare professional if you have concerns.
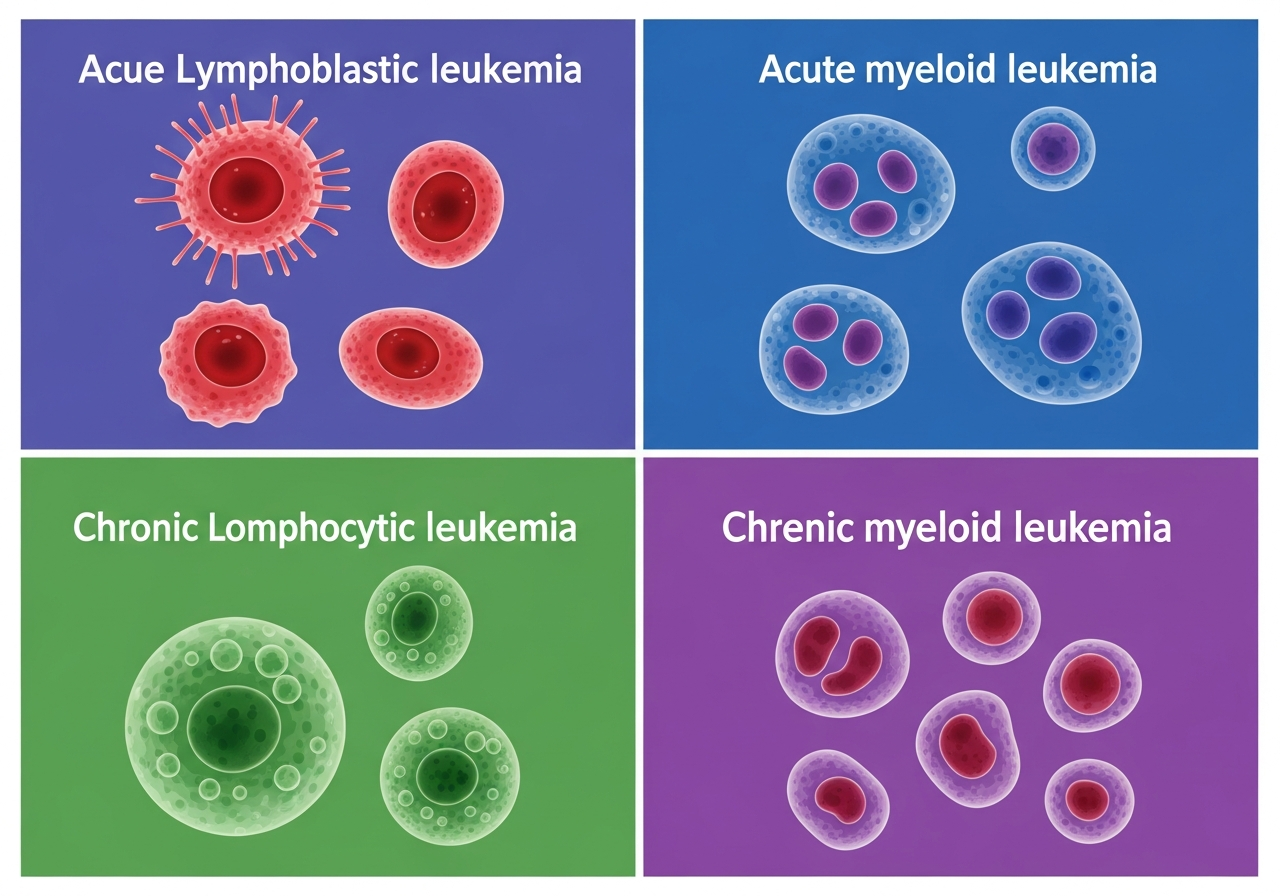
Chronic Myelomonocytic Leukemia (CMML): A Complete Guide
Chronic Myelomonocytic Leukemia (CMML) is a rare hematologic malignancy that occupies a unique clinical and biological space between two broad categories of blood disorders: myelodysplastic syndromes (MDS) and myeloproliferative neoplasms (MPN). Because it shares features with both — it involves dysplastic (abnormally formed) blood cells as in MDS, and overproduction of monocytes as in MPN — it is classified separately under the WHO classification as a "myelodysplastic/myeloproliferative neoplasm" (MDS/MPN).
CMML is primarily a disease of older adults, with a median age at diagnosis of approximately 73 years and a male predominance (2:1 male to female ratio). It is rare, accounting for fewer than 5,000 cases per year in the United States. Despite its rarity, CMML is clinically important because it carries a significant risk of transformation to acute myeloid leukemia (AML) — occurring in approximately 15–30% of patients — and because its treatment options are limited compared to other leukemias.
Understanding CMML's relationship to MDS and MPN, its characteristic monocytosis, the limited but available treatment options, and when allogeneic transplantation should be considered are the central clinical questions in managing this disease.
The Biology of CMML
The defining biologic feature of CMML is the clonal proliferation of monocyte precursors, resulting in a persistent elevation of monocytes (monocytosis) in the peripheral blood. By WHO definition, CMML requires a sustained absolute monocyte count of ≥1,000 cells/μL (some centers use ≥500/μL with appropriate immunophenotypic confirmation), with monocytes comprising ≥10% of total white blood cells.
The molecular pathogenesis of CMML involves a complex landscape of somatic mutations that accumulate in a hematopoietic stem cell. Unlike CML — which is defined by a single, specific translocation (BCR-ABL1) — CMML has no single defining molecular lesion. The most commonly mutated genes in CMML include:
- TET2: Mutated in ~60% of CMML cases; involved in DNA methylation regulation
- SRSF2: An RNA splicing factor gene; mutated in ~40–50%; strongly associated with CMML
- ASXL1: Chromatin modifier; mutated in ~40%; associated with worse prognosis
- RAS pathway genes (KRAS, NRAS): Mutated in ~30–40%; associated with proliferative features and poor prognosis
- CBL: Ubiquitin ligase; mutated in ~10%; associated with myeloproliferative features
- RUNX1: Transcription factor; mutation associated with AML transformation risk
The absence of the Philadelphia chromosome (BCR-ABL1) is required to distinguish CMML from CML in cases of monocytosis with leukocytosis — this is an important diagnostic distinction that significantly changes management.
CMML Classification: CMML-1 vs. CMML-2
WHO classifies CMML into two subtypes based on blast percentage — a critical distinction because higher blast counts correlate with more aggressive disease and higher AML transformation risk:
- CMML-1: Peripheral blood blasts <5% AND bone marrow blasts <10%
- CMML-2: Peripheral blood blasts 5–19% OR bone marrow blasts 10–19% (or presence of Auer rods at any blast percentage)
Additionally, CMML can be phenotypically categorized based on whether the proliferative (MPN-like) or dysplastic (MDS-like) features predominate:
- Proliferative CMML: WBC ≥13,000/μL; more constitutional symptoms; larger spleens; higher rate of RAS pathway mutations; associated with higher transformation risk
- Dysplastic CMML: WBC <13,000/μL; more cytopenias; less prominent splenomegaly
Symptoms of CMML
CMML symptoms reflect its dual MDS/MPN nature — a combination of cytopenia-related symptoms and proliferative features:
- Constitutional symptoms: Fatigue, weight loss, night sweats, and low-grade fever are common and often the first symptoms prompting medical evaluation
- Splenomegaly: Abdominal fullness and early satiety from splenic enlargement — more prominent in proliferative CMML
- Anemia: Fatigue, pallor, breathlessness from impaired red blood cell production
- Thrombocytopenia: Easy bruising and bleeding risk
- Recurrent infections: From functional immune impairment and neutropenia
- Skin manifestations: CMML can infiltrate the skin, producing leukemia cutis — firm, violaceous skin nodules. Rare but diagnostically important
- Pleural and pericardial effusions: In some proliferative CMML patients, fluid accumulation around the lungs or heart contributes to breathlessness and chest discomfort
Many CMML patients are discovered incidentally when blood work performed for other reasons reveals monocytosis or cytopenias. In some patients, the initial CBC finding is a modest absolute monocyte count elevation without symptoms — leading to the important distinction of "clonal monocytosis of undetermined significance" (CMUS) versus frank CMML.
Diagnosing CMML
CMML diagnosis requires a systematic evaluation to confirm monocytosis, exclude other causes of monocytosis (infectious, inflammatory, and other hematologic conditions), and characterize the disease molecularly:
- CBC with differential: Persistent absolute monocytosis (≥1,000/μL) with monocytes ≥10% of WBCs. Variable anemia and thrombocytopenia. May have a mild leukocytosis. About blood tests in leukemia.
- Peripheral blood smear: Monocytes should be counted carefully — in CMML, monocytes are predominantly classical monocytes (CD14+CD16-) on flow cytometry (>94%), distinguishing them from monocytosis in reactive conditions where intermediate and non-classical monocytes predominate.
- Flow cytometry (peripheral blood): Classical monocyte partition ≥94% is now recognized as a strong diagnostic criterion for clonal CMML monocytosis.
- BCR-ABL1 PCR/FISH: Must be negative to exclude CML.
- Bone marrow biopsy: Confirms dysplastic changes, blast percentage (CMML-1 vs. CMML-2), and rules out other diagnoses. Provides tissue for cytogenetics and molecular testing. About bone marrow biopsy.
- Cytogenetics: Abnormal in ~30% of CMML; del(7q), trisomy 8, and complex karyotype are adverse prognostic features.
- Molecular panel (NGS): TET2, SRSF2, ASXL1, KRAS, NRAS, CBL, RUNX1 — important for diagnosis, prognostication, and (increasingly) treatment planning.
Treatment of CMML
Treatment for CMML is guided by disease phase, symptom burden, pace of progression, and patient fitness. Unlike CML, CMML lacks a single defining molecular target that can be blocked with a specific drug. Current treatment options include:
Observation (Watch and Wait)
For asymptomatic CMML-1 patients with stable, low disease burden and no high-risk features, observation with periodic monitoring (CBC every 3 months, bone marrow re-evaluation annually or with changes) is appropriate. This particularly applies to dysplastic CMML with preserved blood counts and no constitutional symptoms.
Hypomethylating Agents (HMAs)
Azacitidine (Vidaza) and decitabine (Dacogen) are the primary treatment modalities for CMML patients requiring therapy. These are epigenetic agents that inhibit DNA methyltransferase, leading to re-expression of silenced tumor suppressor genes and promoting differentiation of dysplastic cells. HMAs are given in repeated cycles (typically every 28 days, for 6 or more cycles to assess response).
HMAs achieve responses (hematologic improvement, partial remission) in approximately 40–50% of CMML patients. Complete remissions are less common (~15–20%). HMAs can reduce transfusion requirements, improve blood counts, reduce constitutional symptoms, and may delay AML transformation. However, they are not curative and responses are typically maintained only with continued therapy.
Allogeneic Stem Cell Transplantation
The only potentially curative treatment for CMML is allogeneic stem cell transplantation (allo-SCT). Unfortunately, the predominantly older age of CMML patients significantly limits eligibility for transplantation. Reduced-intensity conditioning (RIC) regimens have expanded transplant access to older patients (up to age 70–75 in some centers) with lower treatment-related mortality. Transplantation is generally considered for:
- Younger patients (under 65–70) with high-risk CMML features (CMML-2, adverse cytogenetics, proliferative features, ASXL1/RAS mutations)
- Patients with CMML-2 who are at high risk of imminent AML transformation
- Patients with CMML that has failed HMA therapy with adequate performance status
Supportive Care
Transfusions (red blood cells and platelets), growth factors, and antimicrobials for infections are important components of CMML management, particularly in patients not receiving or not responding to HMA therapy.
Clinical Trials
Given the limited treatment options for CMML, clinical trial participation is strongly encouraged. Current trials investigate novel combinations of HMAs with targeted agents (venetoclax, gilteritinib), IDH inhibitors in IDH-mutated CMML, and novel transplant approaches. See clinical trials and treatment decisions.
Prognosis in CMML
CMML prognosis is variable but generally guarded. Several prognostic scoring systems exist — including CPSS, CPSS-mol, and CMML-specific scoring systems incorporating molecular data. Key prognostic factors:
- Favorable: CMML-1; dysplastic subtype; TET2 mutation without other high-risk mutations; stable low WBC
- Adverse: CMML-2; proliferative subtype; ASXL1 mutation; RAS pathway mutations; adverse cytogenetics (del7q, complex karyotype)
Median survival ranges from approximately 12–30 months depending on risk category. CMML-2 has a higher rate of AML transformation and shorter overall survival. Allogeneic SCT in appropriately selected patients offers the potential for long-term remission.
Patient Considerations
CMML is a rare disease, and patients benefit greatly from being evaluated at centers with specific expertise in MDS/MPN overlap syndromes. Prognostic stratification using modern molecular scoring — which requires comprehensive NGS testing — is essential for treatment planning. Patients should discuss clinical trial options explicitly with their hematologist; many trials are specifically recruiting CMML patients given the limited approved treatment options. Blood transfusion requirements should be managed with iron chelation when cumulative transfusions become excessive, to prevent transfusional iron overload.
Caregiver Guidance
CMML caregivers often support a patient who is older, may have significant comorbidities, and is on a long-term treatment program with regular monitoring. Caregivers should be alert to signs of worsening cytopenias (increasing fatigue, new easy bruising, frequent infections) and to constitutional symptom escalation — which may indicate disease progression or AML transformation requiring urgent re-evaluation. Transportation to regular monitoring appointments and HMA infusion cycles is a practical but essential caregiver responsibility.
When to Seek Medical Attention
- Fever above 101°F in any CMML patient — infection risk is significant
- Rapid worsening of fatigue, pallor, or breathlessness — possible accelerating anemia
- New or rapidly increasing bruising and bleeding — thrombocytopenic complication
- Sudden onset of AML-like acute symptoms — possible blast transformation
- Severe left-sided abdominal pain — splenic event in the context of splenomegaly
🚨 When CMML Patients Need Urgent Care
- Fever above 101°F — immune compromise makes infection serious
- Sudden severe fatigue, bleeding, or rapidly worsening symptoms — possible AML transformation
- Severe abdominal pain in a patient with known splenomegaly
💬 Questions to Ask Your CMML Healthcare Team
- What is my CMML classification (CMML-1 vs. CMML-2) and what mutations were found?
- What is my CMML prognostic risk category and what does it predict?
- Do I need treatment now, or is observation appropriate?
- Am I a candidate for allogeneic stem cell transplantation?
- Are there clinical trials available for my CMML?
- How will you monitor for AML transformation, and what signs should prompt an earlier evaluation?
This content is for informational and educational purposes only. It is not a substitute for professional medical advice, diagnosis, or treatment. Always consult your physician or a qualified healthcare provider with any questions about a medical condition. Never disregard professional medical advice or delay seeking it because of information you have read on this website. Read our full disclaimer.
Frequently Asked Questions
Yes — CMML is a rare blood cancer that features characteristics of both myelodysplastic syndromes (MDS) and myeloproliferative neoplasms (MPN).
CMML lacks the Philadelphia chromosome that defines CML and specifically involves overproduction of monocytes rather than granulocytes.
Options include hypomethylating agents (azacitidine, decitabine), supportive care, and allogeneic stem cell transplant for eligible patients.
