📋 Quick Summary
- Topic: Chromosomal abnormalities, inherited vs. acquired mutations, genetic testing, and what these mean for patients and families.
- Key Takeaway: Early recognition and medical consultation are critical for the best clinical outcomes.
- Remember: Always consult a qualified healthcare professional if you have concerns.
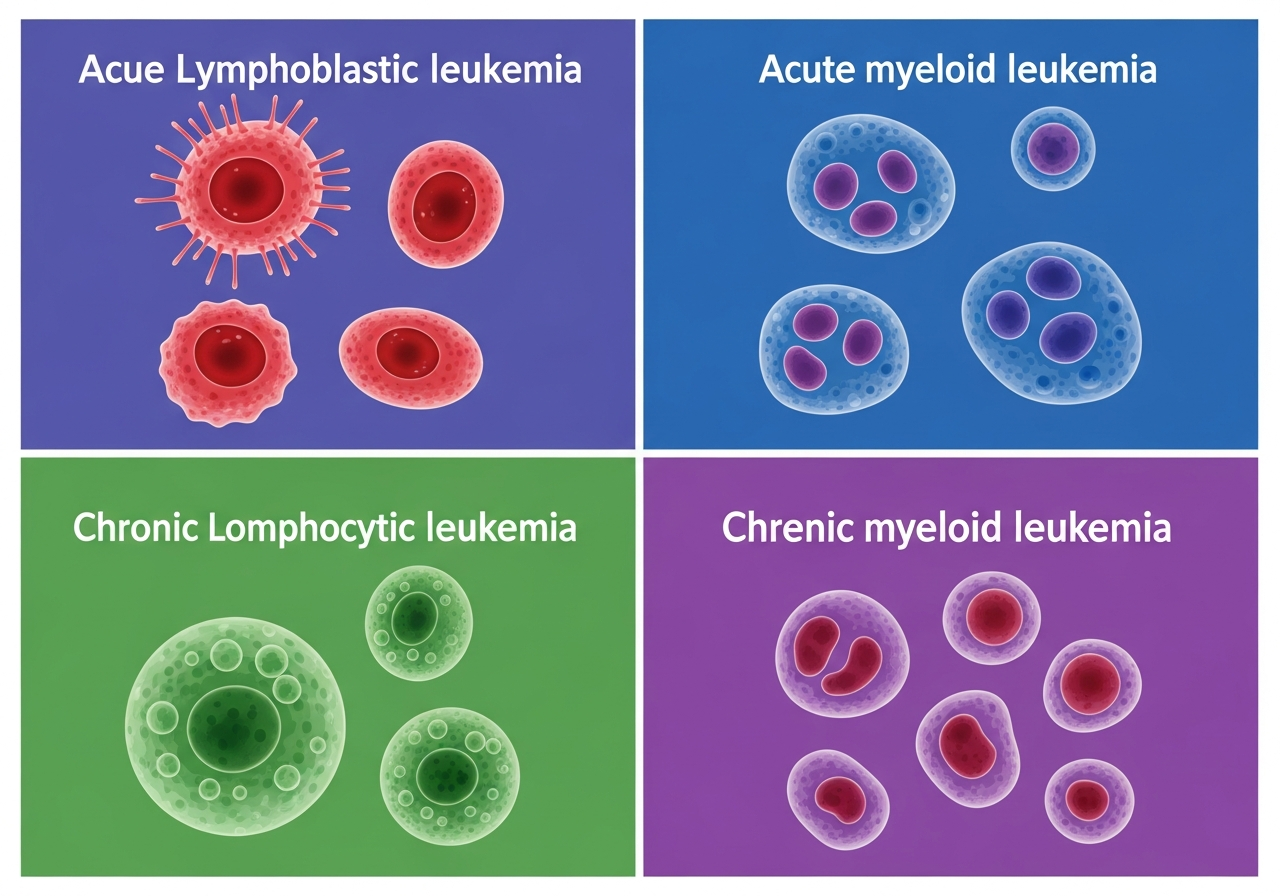
The Genetics of Leukemia: What Patients Need to Know
Leukemia is fundamentally a genetic disease — it arises from accumulated mutations in the DNA of a blood-forming stem cell that alter normal regulatory processes, driving uncontrolled proliferation. Understanding the genetics of leukemia is not merely an academic exercise: the specific genetic and chromosomal abnormalities found in a patient's leukemia cells determine the type and subtype of disease, guide treatment selection, inform prognosis, and — in a minority of cases — have implications for other family members who may share inherited predisposing genetic variants. Genetic profiling is now central to how each leukemia type is classified and treated — from the Philadelphia chromosome that defines CML to the FLT3 and NPM1 mutations that risk-stratify AML.
This article explains the key genetic concepts in leukemia: the difference between acquired (somatic) and inherited (germline) mutations, the major chromosomal abnormalities and gene mutations that characterize different leukemia types, the role of genetic counseling, and how genetics connects to treatment decisions across the full spectrum of leukemia types and subtypes. How these results are interpreted is explained in our guide to understanding leukemia test results.
Acquired vs. Inherited Genetic Mutations: A Critical Distinction
One of the most important concepts for leukemia patients and families to understand is the distinction between somatic (acquired) mutations and germline (inherited) mutations:
Somatic (Acquired) Mutations
The vast majority of genetic abnormalities found in leukemia cells are somatic — meaning they are acquired during the patient's lifetime, arising in a single blood-forming cell and then clonally passed to all of that cell's daughter leukemia cells. Somatic mutations are:
- Present ONLY in the leukemia cells — not in normal tissue cells of the same patient
- NOT inherited from parents
- NOT transmitted to children
- NOT a risk factor for blood relatives
BCR-ABL1 in CML, FLT3 mutations in AML, NPM1 mutations in AML, and TP53 mutations in CLL are all, in most cases, somatic mutations. Finding these in a patient's leukemia cells does not mean that their children or siblings are at increased risk of leukemia. It is essential that oncologists communicate this clearly to patients, who often fear — unnecessarily — that they have "passed leukemia" to their children. The risk of leukemia across life stages is shaped by a combination of genetic predisposition and environmental exposures — not a simple inherited blueprint.
Germline (Inherited) Mutations
A minority of leukemia cases — perhaps 5–10% — are associated with a germline predisposition: an inherited mutation in a cancer-susceptibility gene that was present in every cell of the patient's body from conception and that may be present in blood relatives. Unlike somatic mutations, germline variants:
- Are present in ALL cells — blood, skin, saliva — not just leukemia cells
- May be inherited from one or both parents
- May be transmitted to children (50% risk with autosomal dominant inheritance)
- May have implications for other family members who could benefit from screening or preventive monitoring
Germline predisposition genes relevant to leukemia include RUNX1, GATA2, DDX41, CEBPA, TP53 (Li-Fraumeni syndrome), BRCA2, PALB2, and others. These are increasingly important as NGS testing identifies germline variants — distinguishing somatic from germline requires testing of non-tumor tissue (typically saliva or skin fibroblasts) to confirm whether a variant is present in normal cells.
Key Chromosomal Abnormalities in Leukemia
Chromosomal rearrangements are the most dramatic genetic changes in leukemia and serve as defining markers for specific subtypes:
| Abnormality | Leukemia Type | Created Gene Fusion | Significance |
|---|---|---|---|
| t(9;22) — Philadelphia chromosome | CML; Ph+ ALL | BCR-ABL1 | Defining for CML; TKI target; high-risk in ALL |
| t(15;17) | APL (AML-M3) | PML-RARA | Defining for APL; highly treatable with ATRA+ATO |
| t(8;21) | AML | RUNX1-RUNX1T1 | Favorable; excellent response to standard chemotherapy |
| inv(16)/t(16;16) | AML (M4 eos) | CBFB-MYH11 | Favorable; eosinophilia; HiDAC consolidation |
| del(17p) / TP53 loss | CLL; AML | TP53 loss of function | Very poor prognosis; resistance to chemo; BTKi/venetoclax for CLL |
| del(13q) | CLL | DLEU2/miR-15a/16-1 loss | Favorable (if isolated); many patients never need treatment |
| Hyperdiploidy (>50 chromosomes) | B-ALL (childhood) | Multiple trisomies | Very favorable; excellent MTX response; cure rates >95% |
| KMT2A (MLL) rearrangements | Infant ALL; AML; T-ALL | KMT2A-MLLT3, etc. | High-risk; poor prognosis; clinical trial priority |
Key Gene Mutations in Leukemia
Beyond chromosomal rearrangements, point mutations and small insertions/deletions (indels) in specific genes are critical drivers and biomarkers in leukemia:
- FLT3 (AML): Internal tandem duplications (ITD) in FLT3 are found in ~25–30% of AML. FLT3-ITD confers increased proliferative drive and historically poor prognosis. FLT3 TKD mutations occur in ~5–10%. Both are now targeted with midostaurin (1L) and gilteritinib (R/R).
- NPM1 (AML): Mutated in ~30% of AML. Alone (without FLT3-ITD), NPM1 mutation confers favorable prognosis. Also a highly sensitive MRD marker.
- IDH1/IDH2 (AML): Isocitrate dehydrogenase mutations in ~20% of AML. Produce an oncometabolite (2-hydroxyglutarate) that impairs differentiation. Targetable with ivosidenib (IDH1) and enasidenib (IDH2).
- TP53 (AML, CLL, ALL): The most common tumor suppressor gene mutated in human cancer. In leukemia, TP53 mutation/deletion confers resistance to most chemotherapy and targeted agents and very poor prognosis. Novel approaches under investigation include APR-246 (refolding mutant p53), MDM2 inhibitors, and immune approaches.
- RUNX1 (AML, ALL): Frequent in therapy-related AML and de novo AML; poor prognosis with standard therapy. Also important germline predisposition gene (RUNX1 familial platelet disorder).
- NOTCH1/FBXW7 (T-ALL): Activating mutations in ~50–60% of T-ALL; may confer better prognosis in T-ALL context.
- KRAS/NRAS (AML, CMML): RAS pathway mutations drive proliferation; more common in CMML and pediatric AML. Targeted MEK inhibitors under investigation.
- SRSF2/SF3B1/U2AF1 (MDS, CMML): RNA splicing factor mutations; strongly associated with myelodysplastic phenotype. SF3B1 mutation specifically associated with ringed sideroblasts and favorable prognosis in MDS.
Hereditary Leukemia Predisposition Syndromes
A growing number of inherited predisposition syndromes are recognized as increasing leukemia risk. Recognition of these syndromes has important implications for the patient, their treatment (particularly SCT donor selection — family members who share the germline mutation are not appropriate donors), and family members who may benefit from screening:
- Li-Fraumeni syndrome (germline TP53): Very high lifetime risk of multiple cancers including AML; autosomal dominant; annual screening recommended
- RUNX1 familial platelet disorder: Autosomal dominant germline RUNX1 mutation; platelet dysfunction; ~35% lifetime risk of AML
- GATA2 deficiency: Autosomal dominant; immunodeficiency; high risk of MDS/AML; lymphedema
- Fanconi anemia: Autosomal recessive; DNA repair defect; very high risk of AML and solid tumors; requires modified chemotherapy protocols
- Down syndrome (trisomy 21): 10–20x increased ALL risk; 500x increased AML risk; specific leukemia subtypes respond well to standard therapy
- Noonan syndrome (germline PTPN11, SOS1 others): Associated with juvenile myelomonocytic leukemia (JMML) in childhood
- DDX41 germline mutations: Autosomal dominant; increasingly recognized as a relatively common cause of familial MDS/AML in older adults (median age 50+)
Genetic Counseling and Germline Testing
Genetic counseling is recommended when any of the following are present:
- Leukemia or other blood cancers in two or more first-degree relatives
- Leukemia diagnosis at an unusually young age
- Personal or family history of other cancers consistent with a hereditary cancer syndrome
- Physical features associated with a predisposition syndrome (lymphedema, immunodeficiency, platelet dysfunction)
- NGS testing identifies a TP53, RUNX1, DDX41, GATA2, or other potential germline variant — requiring germline testing of non-tumor tissue to confirm
Genetic counselors at cancer centers help patients navigate the implications of germline findings for themselves and their families, including the decision about whether to share information with relatives. For patients pursuing allogeneic SCT, identifying germline mutations is critical — family members who share the same mutation should not serve as stem cell donors.
Diagnostic Use of Genetics
Genetic testing is central to leukemia diagnosis and classification. The bone marrow biopsy provides material for cytogenetic analysis and molecular testing. The results — karyotype, FISH panel, NGS mutation panel, and (where applicable) PCR for specific gene fusions — together define the WHO classification and the ELN (for AML) or iwCLL/NCCN (for CLL) risk category that drives all subsequent treatment decisions.
Genetics-Guided Treatment
The use of genetic data to select treatment is the defining principle of precision oncology in leukemia. The full landscape of targeted therapies, immunotherapy, chemotherapy selection, and transplant decisions are discussed in the dedicated treatment guides. The key principle is: no treatment decision should be made without complete molecular characterization.
How Genetics Determines Prognosis
Molecular features are the strongest determinants of leukemia prognosis. In AML, ELN risk classification based on cytogenetics and gene mutations predicts 5-year survival ranging from 10% (adverse risk) to >90% (APL). In CLL, del(17p)/TP53 mutation predicts rapid progression requiring immediate targeted therapy. In ALL, Philadelphia chromosome status determines whether a TKI is needed and guides transplant decisions. Understanding one's specific genetic risk category — and the treatment implications — is the most actionable piece of information a leukemia patient can have.
Patient Considerations
Patients should receive a written summary of their molecular findings, risk category, and how these influenced treatment selection. This document should be maintained as a permanent medical record — it will be needed by any future provider. Patients with potential germline variants should be referred for formal genetic counseling before making decisions about family member screening. See clinical trials for information on how genetic subtype affects trial eligibility.
Caregiver and Family Guidance
If the oncology team mentions a possible "hereditary" or "germline" component to the leukemia, family members should discuss with the team whether they should pursue genetic counseling or testing. This is particularly important before any family member is considered as a stem cell donor — a family member carrying the same predisposing mutation should not donate marrow or peripheral blood stem cells. Caregivers should ask explicitly: "Has germline testing been recommended, and should any family members be seen by a genetic counselor?"
When to Seek Medical Attention
Genetic information generally affects long-term management rather than acute care decisions. However, patients with known high-risk genetic profiles (TP53-mutated leukemia, del(17p) CLL) should maintain especially close follow-up and should seek immediate evaluation for any acute symptom escalation — these subtypes can transform or progress rapidly. For acute symptoms (fever, bleeding, breathlessness, neurological changes), immediately seek emergency care as described throughout this site.
🚨 Universal Leukemia Emergency Signs
- Fever above 101°F — regardless of genetic subtype, febrile neutropenia is always an emergency
- Uncontrolled bleeding
- Sudden neurological changes or severe headache
- Rapid symptom escalation in any known high-risk leukemia subtype
💬 Questions to Ask About the Genetics of Your Leukemia
- What genetic and chromosomal abnormalities were found in my leukemia, and what do they mean?
- Are any of these mutations somatic (in the leukemia only) or could they be germline (inherited)?
- Should I or my family members see a genetic counselor?
- Do any of my genetic findings affect who in my family can be a stem cell donor?
- Is there a specific targeted drug approved for my mutation?
- How do my genetics affect my prognosis with standard treatment?
This content is for informational and educational purposes only. It is not a substitute for professional medical advice, diagnosis, or treatment. Always consult your physician or a qualified healthcare provider with any questions about a medical condition. Never disregard professional medical advice or delay seeking it because of information you have read on this website. Read our full disclaimer.
Frequently Asked Questions
Most leukemia is acquired (not inherited). However, certain rare genetic syndromes like Li-Fraumeni or Fanconi anemia increase risk.
Common acquired mutations include the Philadelphia chromosome (BCR-ABL), FLT3, NPM1, and TP53 — occurring over a person's lifetime.
Generally no, since leukemia is rarely directly inherited. Testing is recommended only when a known familial cancer syndrome is present.
