📋 Quick Summary
- Topic: Platelet dysfunction, easy bruising, bleeding gums, nosebleeds, and the severe risk of DIC in Acute Myeloid Leukemia.
- Key Takeaway: Early recognition and medical consultation are critical for the best clinical outcomes.
- Remember: Always consult a qualified healthcare professional if you have concerns.
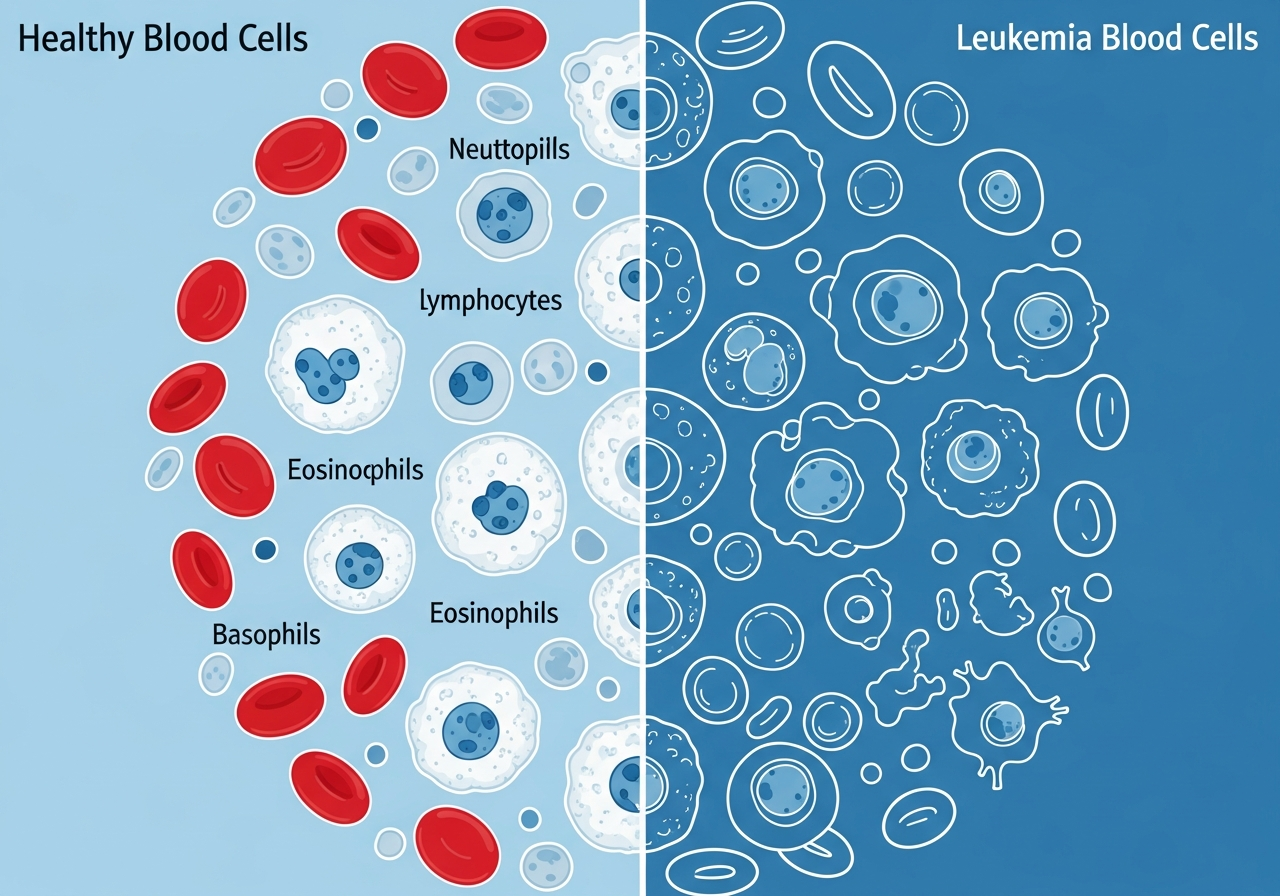
Blood Clotting Problems and Leukemia
Disorders of hemostasis — the body's mechanism for stopping bleeding — are among the most dangerous complications of leukemia. They manifest as a spectrum from mild, cosmetically bothersome bruising and nosebleeds to life-threatening hemorrhage and a catastrophic systemic clotting disorder called Disseminated Intravascular Coagulation (DIC). Understanding the biology of clotting failure in leukemia, recognizing warning signs, and knowing when to seek emergency care can be life-saving. For a broader picture of how bleeding problems fit into the overall symptom picture, visit our leukemia symptoms hub.
The primary driver of clotting problems in leukemia is thrombocytopenia — a severe reduction in platelet count caused by bone marrow failure. Platelets are the small, disc-shaped blood cells that aggregate at sites of vessel injury and form the initial plug that stops bleeding. When platelet counts fall dramatically — as occurs in all types of acute leukemia and in many chronic leukemias — the body's ability to stop even minor bleeds is profoundly impaired. Clotting problems often accompany other hallmark signs such as anemia, extreme fatigue, and increased susceptibility to infections.
Beyond platelet deficiency, some leukemia subtypes — most notably Acute Promyelocytic Leukemia (APL), a subtype of AML — release substances that directly trigger the clotting cascade in a dysregulated fashion, consuming clotting factors and platelets systemically and producing the paradoxical combination of simultaneous clotting and uncontrolled bleeding that characterizes DIC. A complete evaluation begins with blood count testing and often requires a bone marrow biopsy to confirm the underlying leukemia subtype.
How Leukemia Impairs Normal Blood Clotting
Thrombocytopenia: Platelet Production Failure
In a healthy person, the bone marrow produces approximately 150,000–400,000 platelets per microliter of blood, replacing the 150,000 or so that naturally age and are removed from circulation each day. In leukemia, proliferating blast cells crowd the marrow and suppress megakaryopoiesis — the process by which large precursor cells (megakaryocytes) shed platelets into the bloodstream. The result is thrombocytopenia — a platelet count below the normal lower limit of 150,000/μL.
The clinical severity of bleeding risk correlates roughly with platelet count:
- 100,000–150,000/μL: Minimal risk; no spontaneous bleeding; may bleed more than normal with surgery or trauma
- 50,000–100,000/μL: Easy bruising; prolonged bleeding from cuts; increased surgical bleeding risk
- 10,000–50,000/μL: Significant risk of spontaneous bruising; petechiae; nosebleeds; gum bleeding
- Below 10,000–20,000/μL: Spontaneous bleeding into organs (brain, gut, lungs) is possible without any trauma
Platelet Dysfunction
In some leukemias — particularly in CML and myelodysplastic features — the platelets produced are not only fewer in number but also functionally abnormal. These dysfunctional platelets fail to adhere, aggregate, or secrete their contents normally, meaning that even a "normal" platelet count may not provide adequate hemostasis.
Coagulation Factor Deficiencies
In APL specifically, leukemia cells release procoagulant factors (tissue factor and cancer procoagulant) that activate the coagulation cascade throughout the body — consuming clotting factors faster than the liver can synthesize them. The resulting deficiency of factors I (fibrinogen), II, V, VIII, and others renders the patient unable to form stable clots anywhere in the body.
Clinical Signs of Clotting Problems in Leukemia
Bleeding manifestations in leukemia range in severity:
Mild to Moderate Bleeding Signs
- Easy bruising (ecchymosis): Large bruises from minimal or no trauma; appearing in unexpected locations. See our full discussion of leukemia skin changes.
- Petechiae: Pinpoint red dots on the skin, oral mucosa, or conjunctiva from microbleeds. These do not blanch when pressed.
- Prolonged bleeding from cuts: Minor cuts taking 15–30 minutes or more to stop (normal is 1–5 minutes).
- Nosebleeds (epistaxis): Frequent or prolonged — particularly difficult to stop with standard pressure.
- Bleeding gums: Gums bleed during normal tooth brushing; minor dental procedures cause disproportionate bleeding.
- Heavy menstrual periods: Women with leukemia and thrombocytopenia frequently experience significantly heavier menstrual flow.
Severe Bleeding Signs
- Gastrointestinal bleeding: Blood in stool (melena — dark, tarry stool, or hematochezia — bright red blood per rectum); blood in vomit (hematemesis).
- Hematuria: Blood in urine, giving it a pink, red, or brown color.
- Intracranial bleeding: The most feared complication — manifests as sudden severe headache, neurological deficits, confusion, or loss of consciousness. This is a life-threatening emergency.
- Pulmonary hemorrhage: Coughing up blood (hemoptysis); respiratory distress.
- Retinal hemorrhage: Bleeding into the eye causing visual disturbance or floaters.
Disseminated Intravascular Coagulation (DIC): The Critical Emergency
DIC is the most dangerous clotting complication of leukemia and represents a genuine hematologic emergency. It is most commonly associated with Acute Promyelocytic Leukemia (APL, AML-M3), though it can occur in other AML subtypes and in sepsis complicating any leukemia.
What Is DIC?
DIC is characterized by simultaneous, systemic activation of both the coagulation system (forming clots in blood vessels throughout the body) and the fibrinolytic system (breaking down clots). The paradoxical result is that while microscopic clots form in capillaries — causing organ ischemia — the massive consumption of clotting factors and platelets in this process leaves the patient profoundly unable to form clots where they are actually needed. Patients bleed from multiple sites simultaneously: from wounds, from venipuncture sites, from the nose, from the gut, and potentially from the brain.
Clinical Presentation of DIC
- Bleeding from multiple simultaneous sites
- Rapidly spreading purpura (large purple skin patches from subcutaneous bleeding)
- Oozing from IV sites and venipuncture sites
- Signs of organ ischemia (confusion, kidney failure, respiratory failure)
- Markedly prolonged PT and PTT on blood tests; very low fibrinogen; elevated D-dimer
APL and DIC: Why Prompt Diagnosis Is Critical
APL (Acute Promyelocytic Leukemia) is unique among AML subtypes in that the leukemia cells contain characteristic granules packed with procoagulant material. When these cells die — whether from disease itself or from treatment — they release their contents into the bloodstream, triggering DIC. This is why APL has historically been associated with a high early mortality from hemorrhage — patients were dying before specific therapy could be started.
The development of All-Trans Retinoic Acid (ATRA) has transformed APL treatment. ATRA promotes differentiation of APL blasts without causing cell lysis, significantly reducing the DIC trigger. When given immediately upon clinical suspicion of APL — before cytogenetic confirmation — ATRA has dramatically reduced early hemorrhagic death. This is why rapid initiation of ATRA upon clinical suspicion of APL is now a standard oncological emergency protocol.
Diagnostic Evaluation of Clotting Problems
When leukemia-associated bleeding is suspected, the key laboratory tests include:
- Platelet count (from CBC): The primary measure. Critical thresholds are discussed above. See our guide to blood tests in leukemia diagnosis.
- Prothrombin time (PT) and International Normalized Ratio (INR): Measures the extrinsic and common coagulation pathway. Prolonged in coagulation factor deficiency and DIC.
- Activated partial thromboplastin time (aPTT): Measures the intrinsic pathway. Also prolonged in DIC and coagulation factor deficiency.
- Fibrinogen: The clottable protein — critically reduced in DIC as it is consumed. A fibrinogen below 100 mg/dL in combination with other findings is diagnostic of DIC.
- D-dimer: A fibrin degradation product — markedly elevated in DIC, reflecting massive fibrinolysis.
- Peripheral blood smear: May show schistocytes (fragmented red blood cells) in microangiopathic processes including DIC.
In a patient newly presenting with suspected APL (any AML with characteristic DIC, or with the specific morphology of hypergranular blasts on smear), ATRA should be started clinically while awaiting cytogenetic confirmation — this is the standard of care given the rapidity with which APL-associated DIC can become fatal.
Treatment of Clotting Problems in Leukemia
Platelet Transfusion
The primary treatment for thrombocytopenic bleeding is platelet transfusion. Most oncology programs transfuse prophylactically at platelet counts below 10,000–20,000/μL to prevent spontaneous intracranial and organ bleeding. Each unit of single-donor apheresis platelets raises the count by approximately 30,000–60,000/μL. In patients with active bleeding, transfusion thresholds are higher (typically below 50,000/μL).
Fresh Frozen Plasma (FFP) and Cryoprecipitate
In DIC or other coagulopathies where clotting factor levels are dangerously low, FFP (which replaces all coagulation factors) and cryoprecipitate (which provides concentrated fibrinogen, factor VIII, and von Willebrand factor) are given alongside platelet transfusions to correct the full hemostatic defect.
Treating the Underlying Leukemia
As chemotherapy achieves remission and the marrow recovers, platelet production resumes and clotting problems resolve. For APL, ATRA combined with arsenic trioxide is now the standard induction regimen and is so effective that APL — historically one of the most lethal acute leukemia subtypes — now has a cure rate approaching 90%.
Prognosis
The prognosis of bleeding complications in leukemia depends entirely on the severity and location of bleeding and on the speed of diagnosis and treatment. Petechiae and easy bruising are cosmetically significant but not immediately life-threatening. Intracranial hemorrhage carries a mortality of 30–60% or higher. In APL, the introduction of ATRA has reduced early hemorrhagic mortality dramatically, and complete remission rates now exceed 90%. Understanding your leukemia subtype — and what that means for your specific bleeding risk — is covered in detail in our guide to leukemia subtypes and treatment differences. Patients and families can also explore the full range of leukemia treatment options available once a diagnosis is established.
Patient Safety During Thrombocytopenia
Patients with very low platelet counts should take specific precautions:
- Use a soft toothbrush and avoid dental flossing during low platelet periods
- Use electric razors — avoid bladed shaving tools that risk cuts
- Avoid contact sports and activities with risk of head trauma
- Avoid aspirin and NSAIDs, which impair platelet function and worsen bleeding risk
- Apply sustained, firm pressure (10–15 minutes minimum) to any cut before seeking further care
- Avoid constipation — straining during bowel movements can trigger rectal or internal bleeding at low platelet counts
- Know your platelet count before any dental, surgical, or invasive procedure
Caregiver Guidance
Caregivers should maintain a safe home environment during periods of thrombocytopenia: secure loose rugs and clutter that could cause falls, keep a well-stocked first aid kit, and know how to apply effective pressure to any wound. Most critically, caregivers should be alert to signs of serious internal bleeding: sudden severe headache ("thunderclap"), confusion or sudden behavioral change, vision changes, or weakness on one side of the body — all of which require immediate emergency evaluation.
When to Seek Emergency Care
- Any bleeding from multiple sites simultaneously — this is a DIC emergency
- Sudden, severe headache unlike any previous headache — possible intracranial bleeding
- Confusion, weakness on one side, slurred speech, or visual changes in a leukemia patient — emergency
- Bleeding from a wound that does not slow after 15–20 minutes of sustained firm pressure
- Blood in vomit, coughing up blood, or blood in stool in a leukemia patient
- Rapidly spreading large purple patches on the skin
- Any bleeding in a patient with APL — requires emergency medical evaluation
🚨 Bleeding Emergencies in Leukemia — Act Immediately
- Sudden severe headache — possible intracranial bleed
- Bleeding from multiple sites simultaneously — possible DIC
- Confusion, weakness, or vision changes with any bleeding
- Any bleeding that will not stop with sustained pressure
- Known APL with any sign of DIC — emergency hospital contact required
💬 Questions to Ask Your Healthcare Team
- What is my current platelet count, and at what level will I receive a transfusion?
- Do I have any coagulation factor deficiencies in addition to low platelets?
- Am I at risk for DIC given my specific leukemia type?
- What activities should I avoid at my current platelet count?
- Which medications should I absolutely avoid because of bleeding risk?
- What bleeding signs at home should cause me to call 911 rather than wait?
This content is for informational and educational purposes only. It is not a substitute for professional medical advice, diagnosis, or treatment. Always consult your physician or a qualified healthcare provider with any questions about a medical condition. Never disregard professional medical advice or delay seeking it because of information you have read on this website. Read our full disclaimer.
Frequently Asked Questions
Leukemia prevents the bone marrow from producing enough normal platelets (thrombocytopenia), which are essential for clot formation.
Bleeding that won't stop after 10–15 minutes of pressure, coughing up blood, or blood in stool or urine requires emergency care.
Disseminated Intravascular Coagulation (DIC) is a life-threatening clotting disorder particularly associated with Acute Promyelocytic Leukemia (APL), a subtype of AML.
